Billing and Collections
Track every dollar from claim submission through final payment with our billing and collections module built into your desktop application with no internet required. Monitor accounts receivable aging, payment trends, denial rates, and collection performance through interactive dashboards running on your local machine. Post payments or import ERA 835 remittance files to match payments to claims. Manage denials with built-in appeal tracking and resolution timelines. Our integrated AI assistant answers coding questions, explains denial codes, and generates reports without sending patient data online. All data is stored locally and HIPAA compliant with no cloud dependency or monthly fees. The Paper Claims and Electronics Software is also included, at no additional cost.
Features
Billing Reports
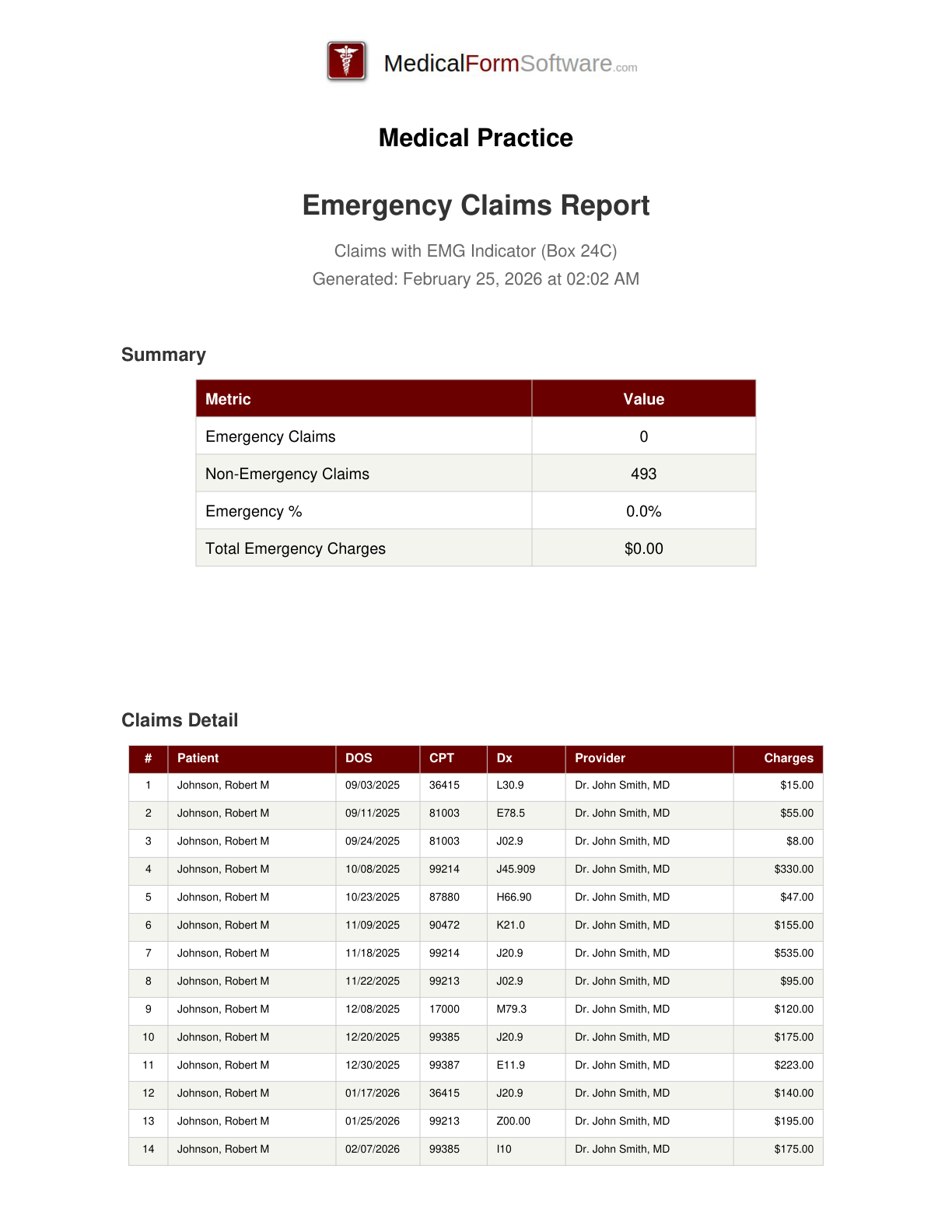
Emergency Claims
Report
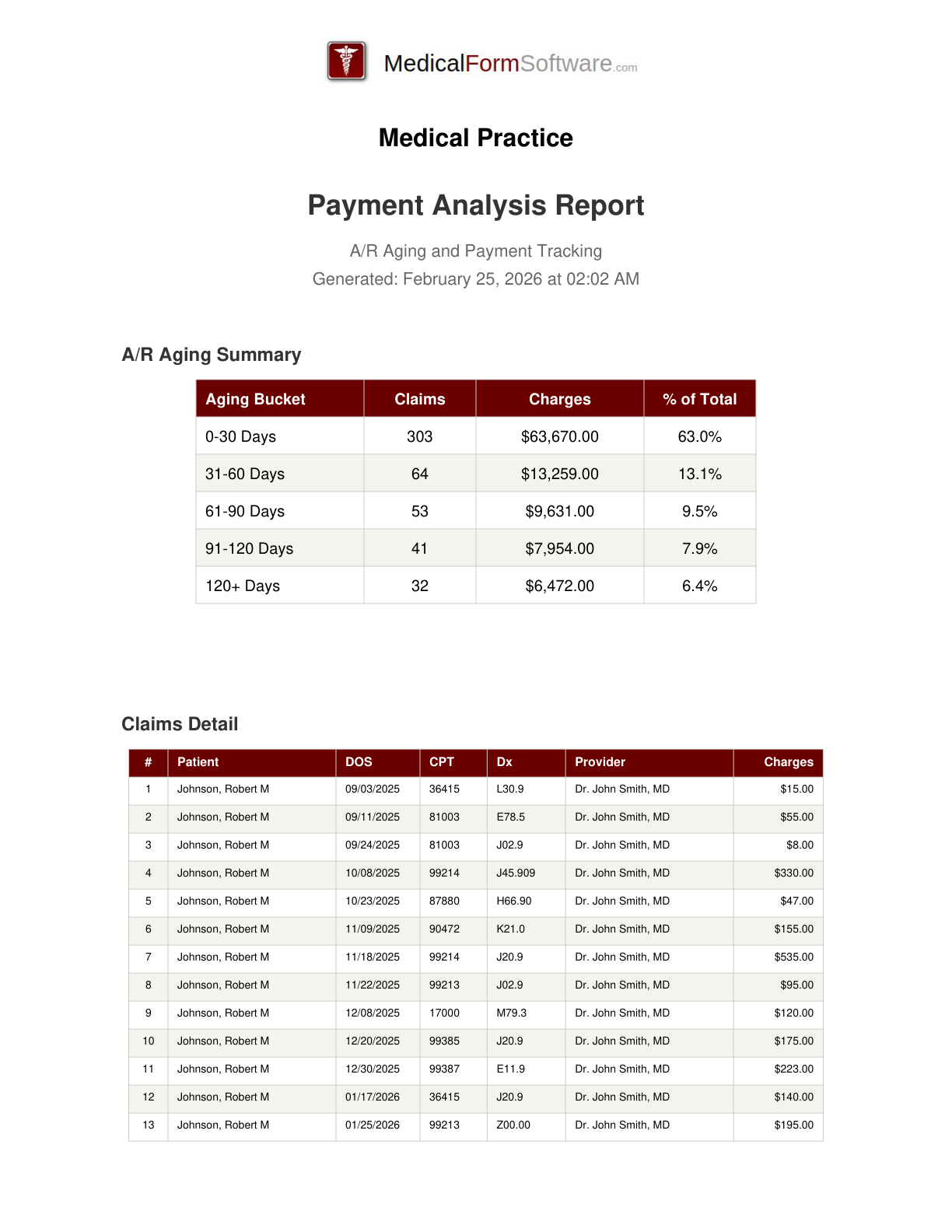
AR Aging
Report
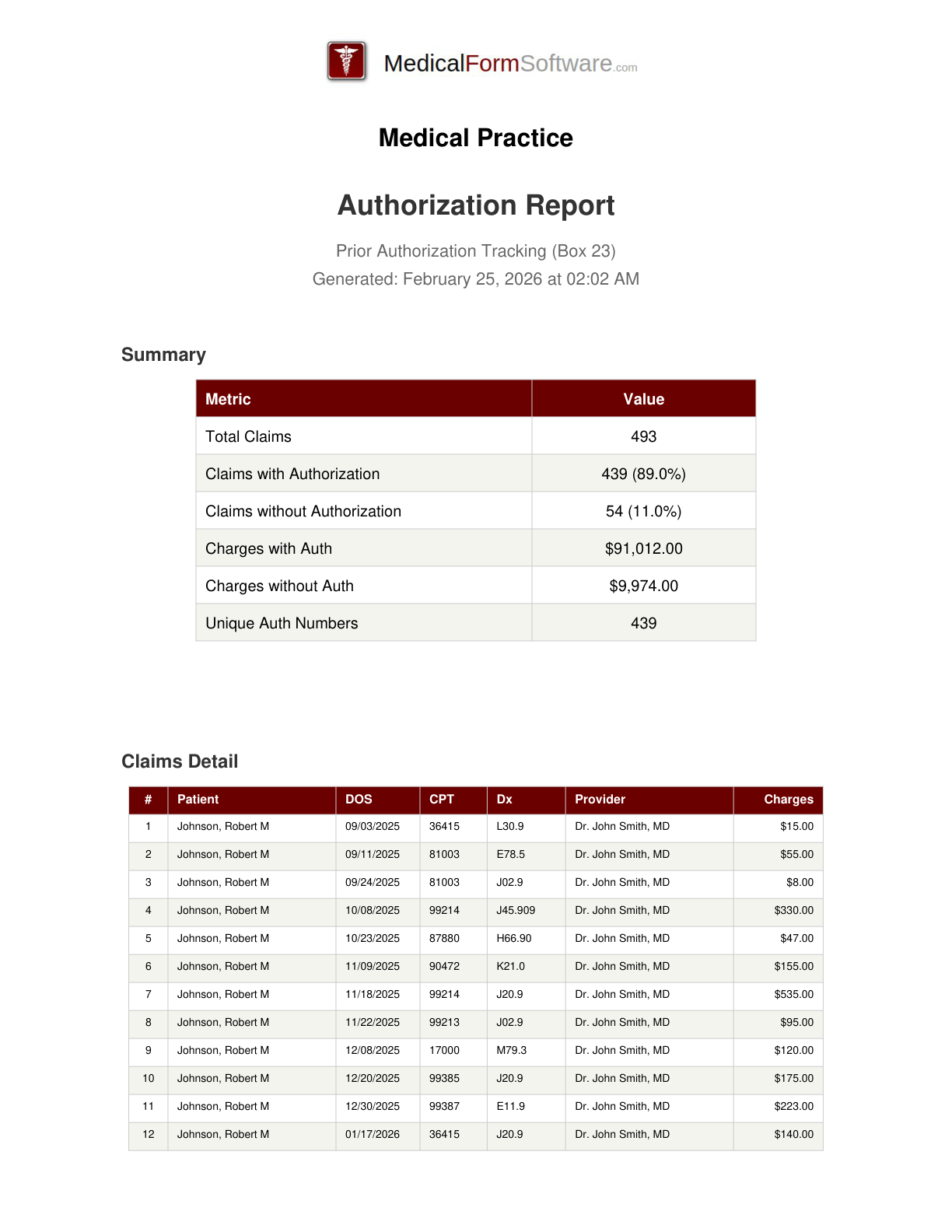
Authorization
Report
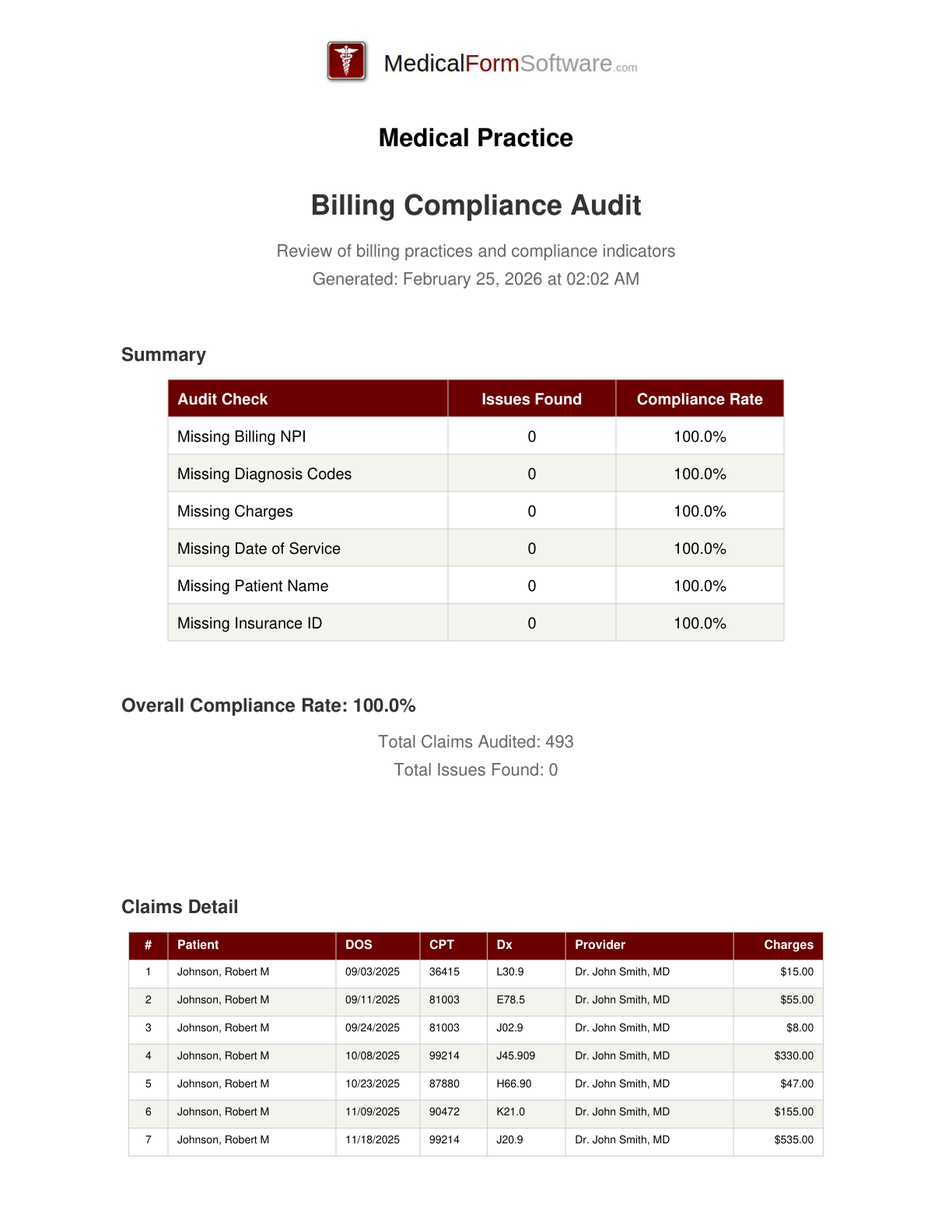
Billing Audit
Report
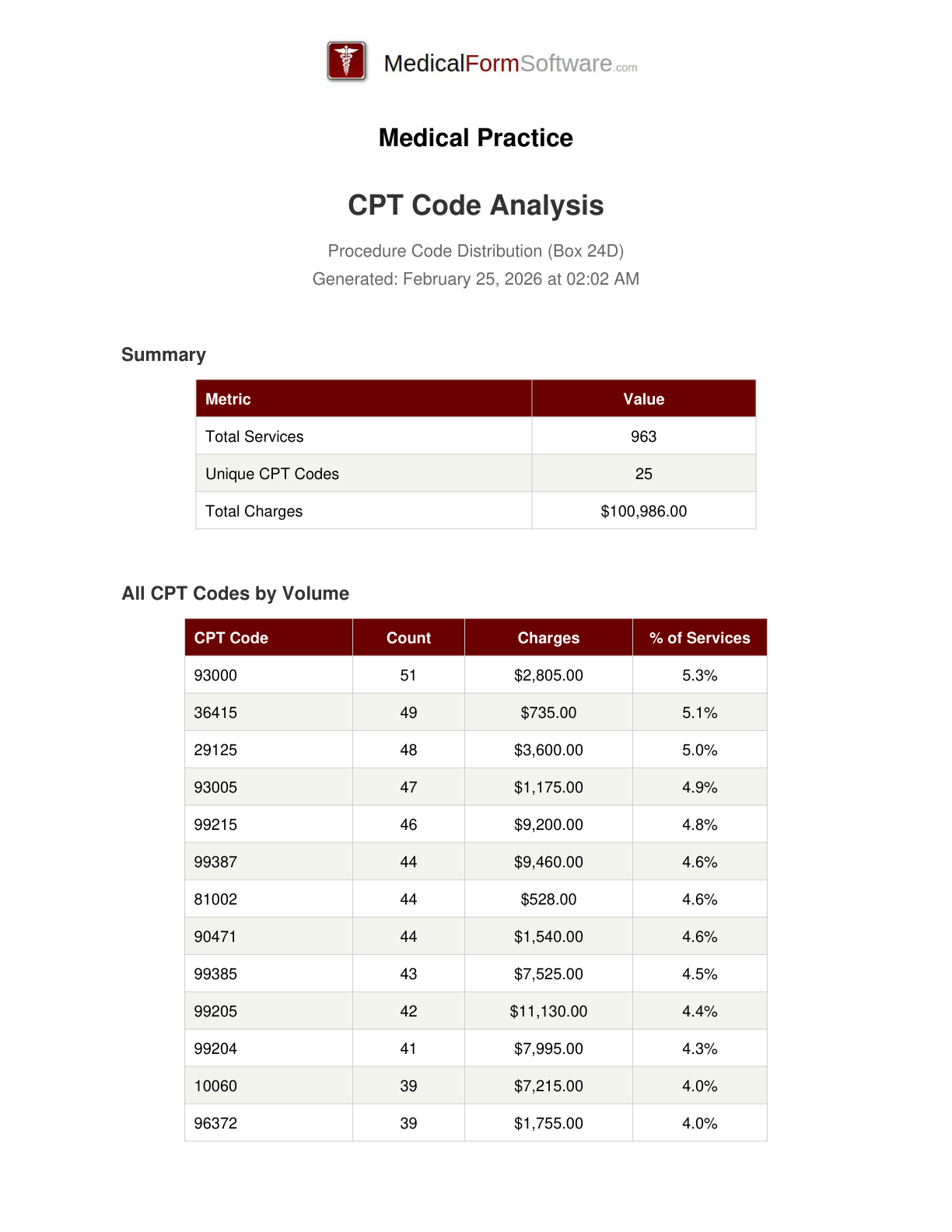
CPT Analysis
Report
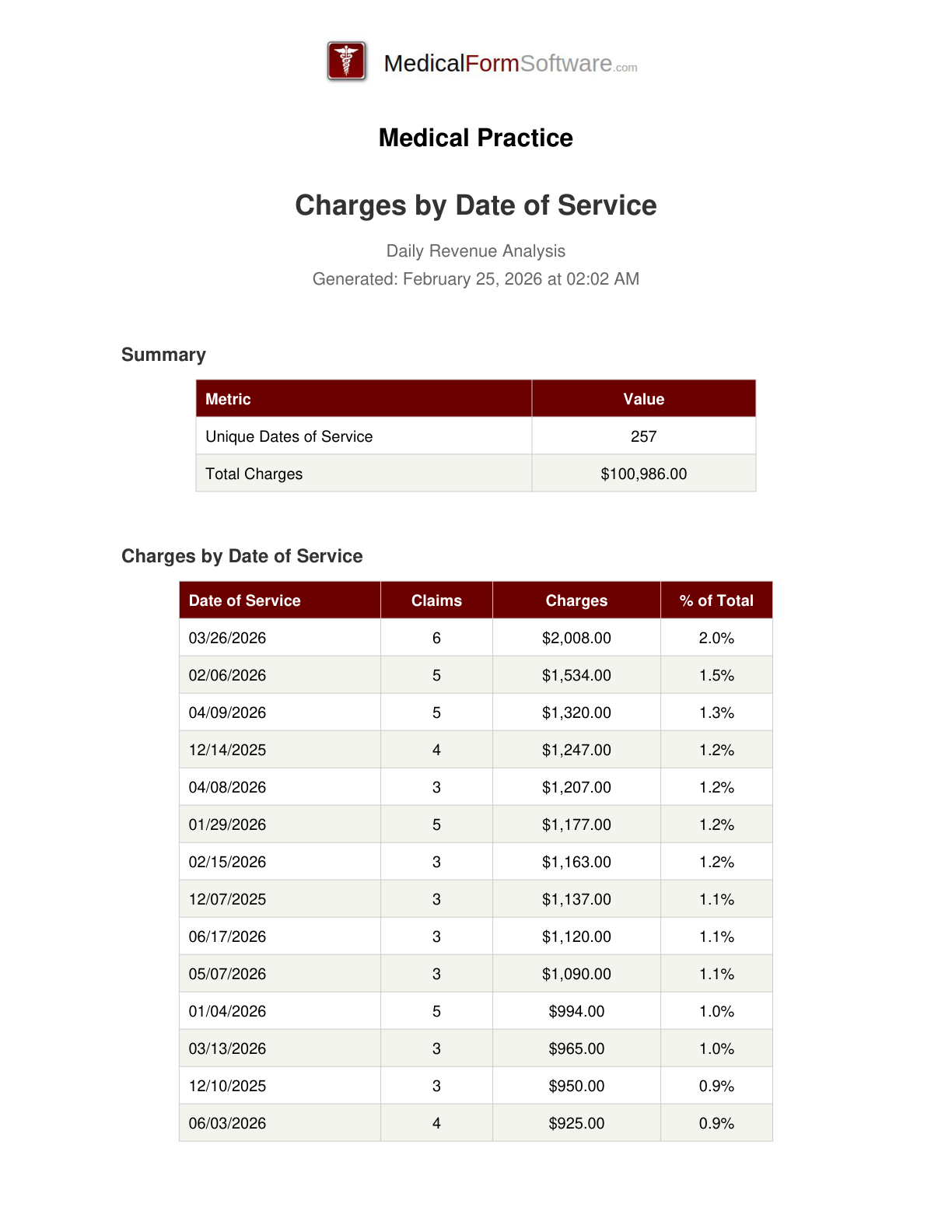
Date of Service
Report
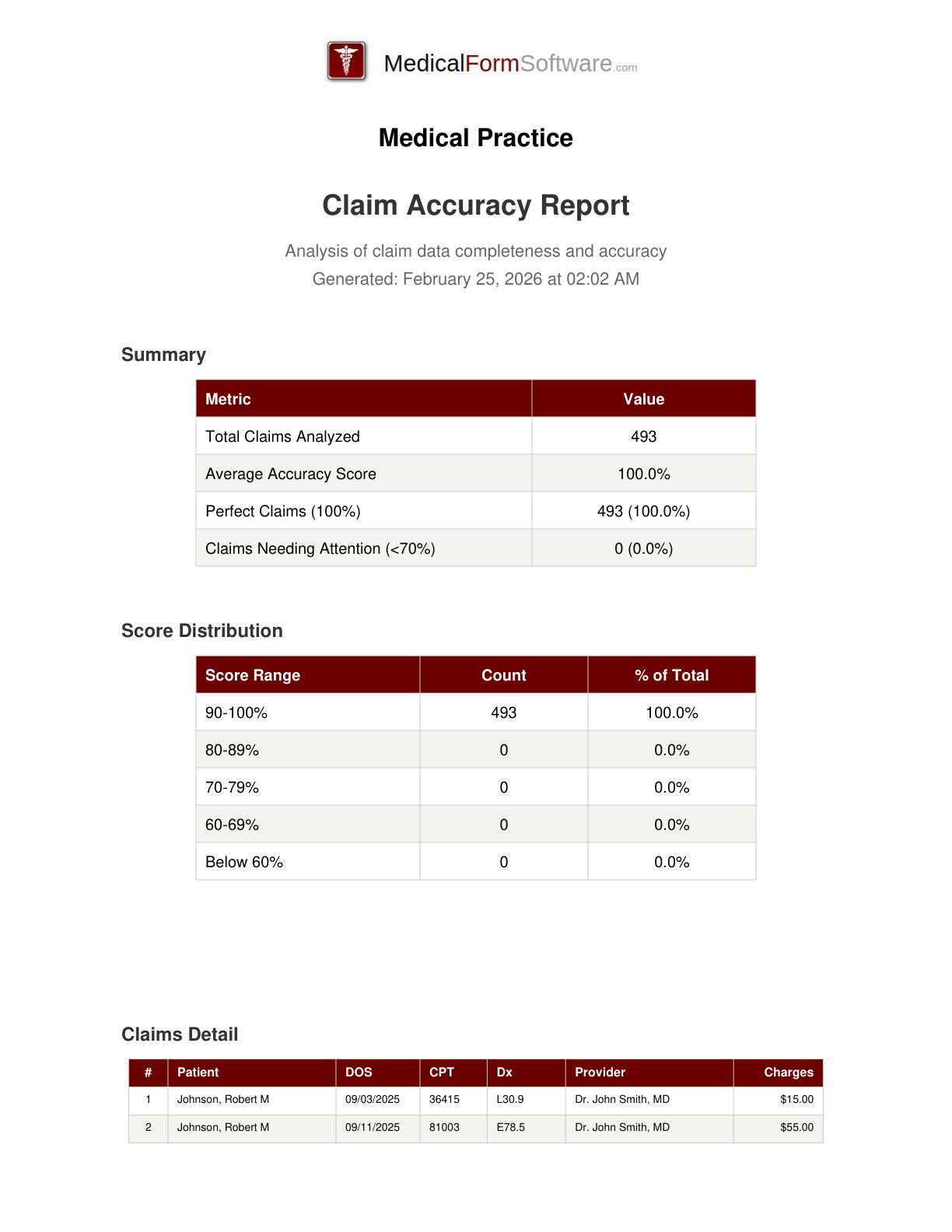
Claim Accuracy
Report
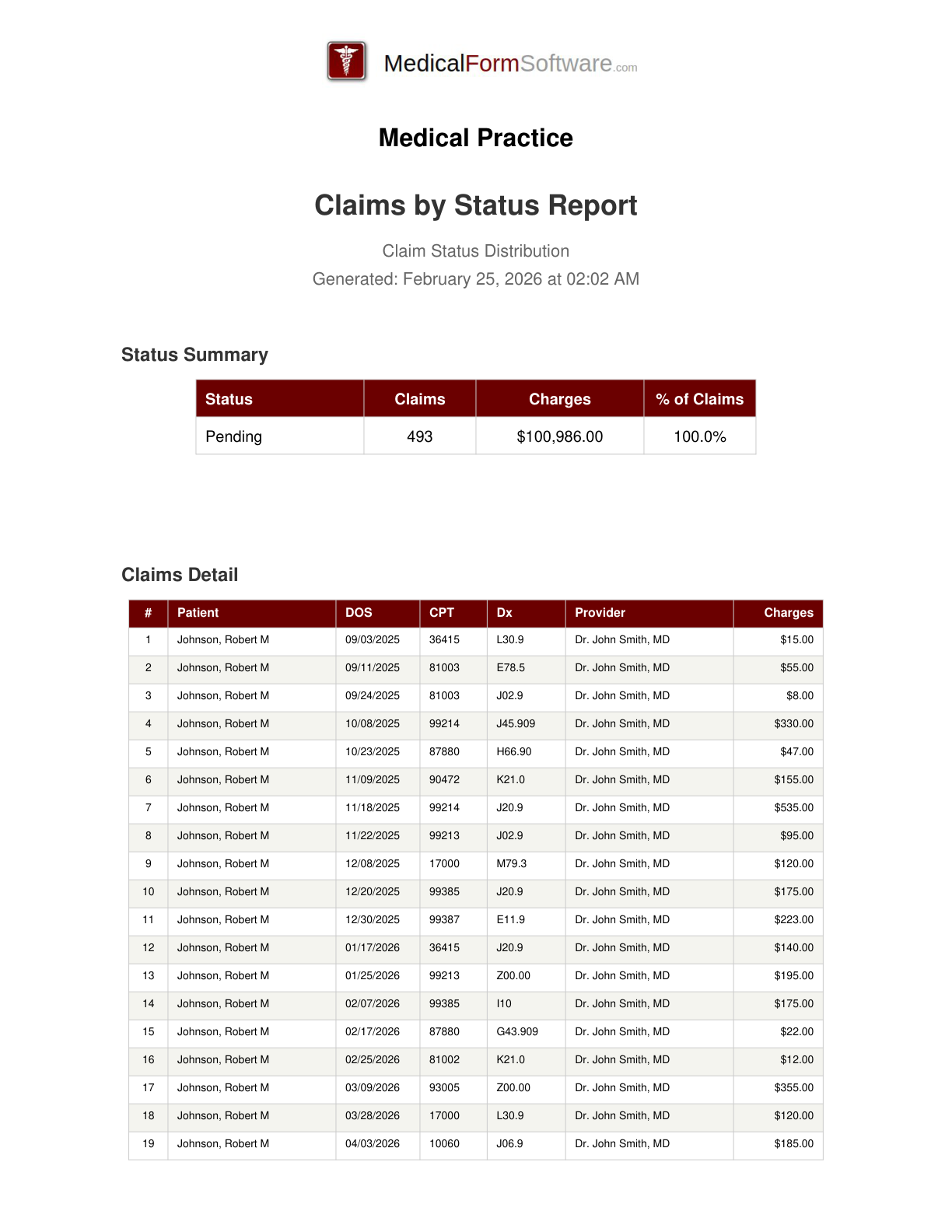
Claim Status
Report
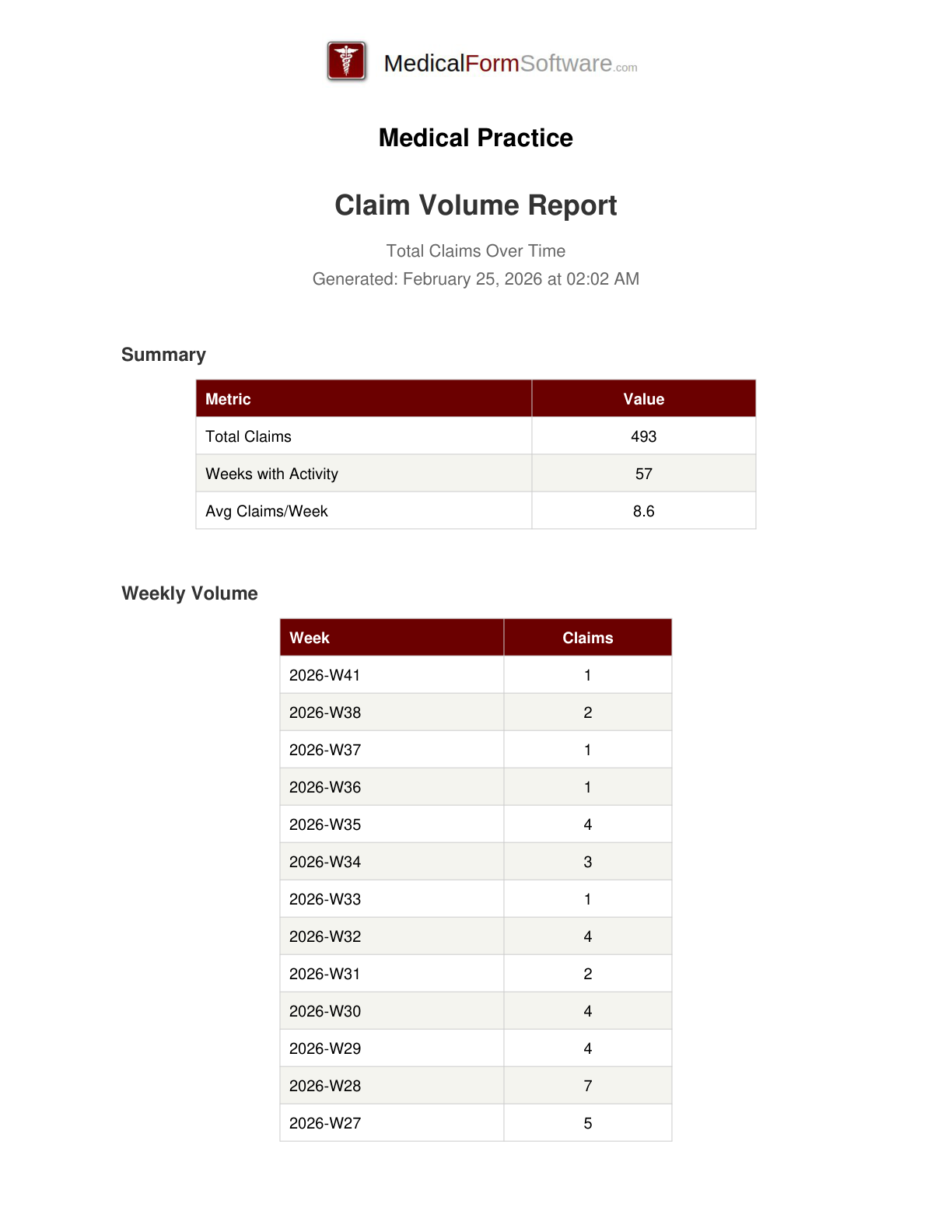
Claim Volume
Report
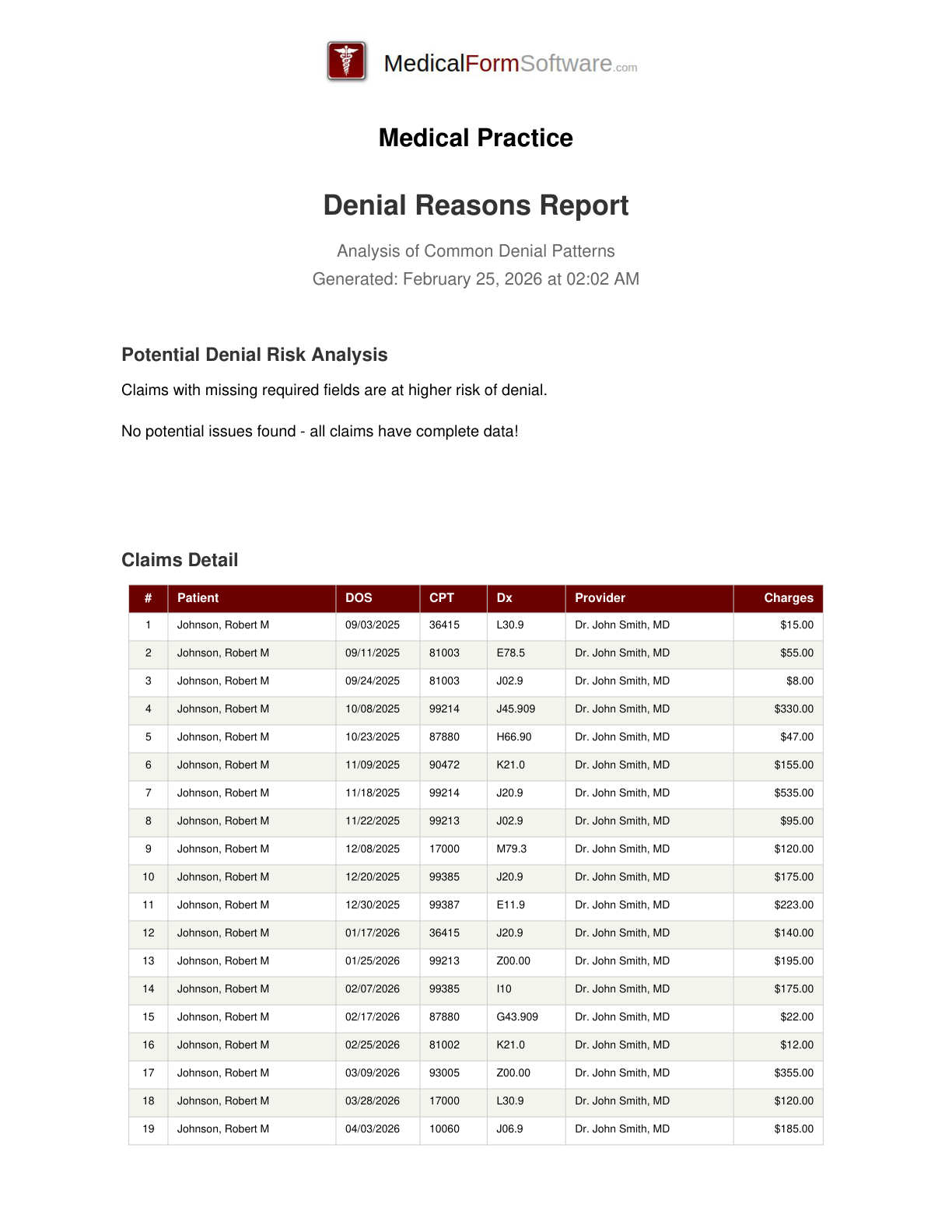
Denial Reasons
Report
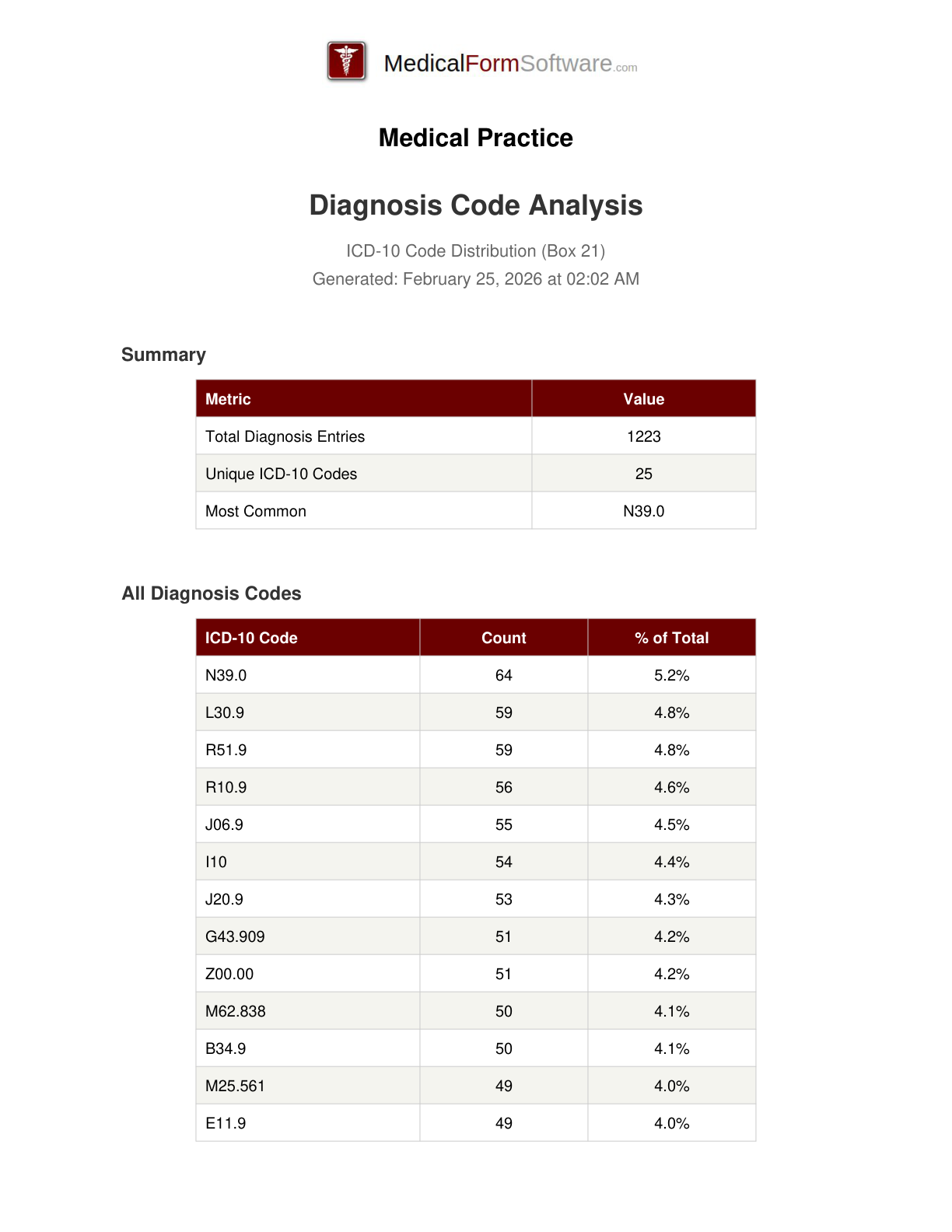
Diagnosis
Report
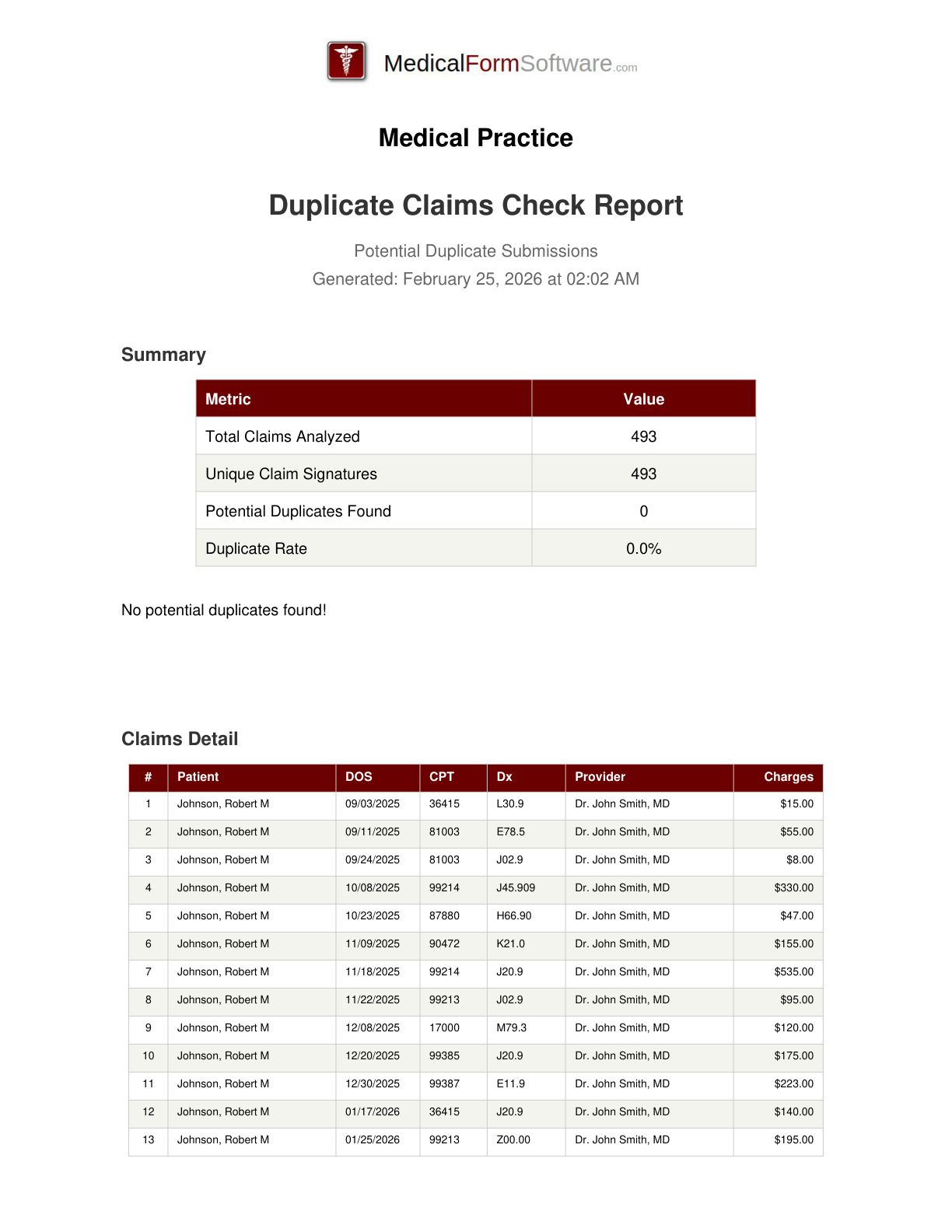
Duplicate Check
Report
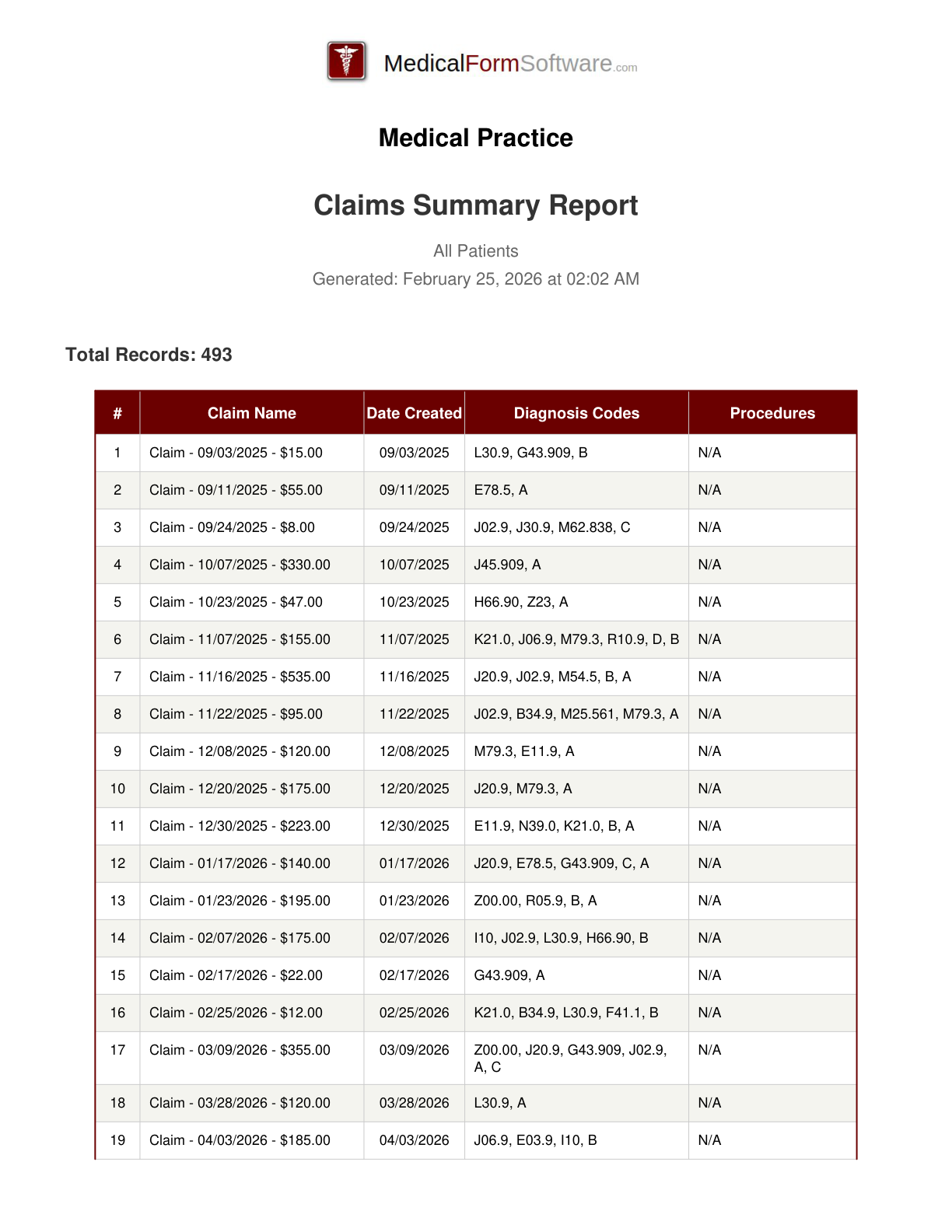
Claims Summary
Report
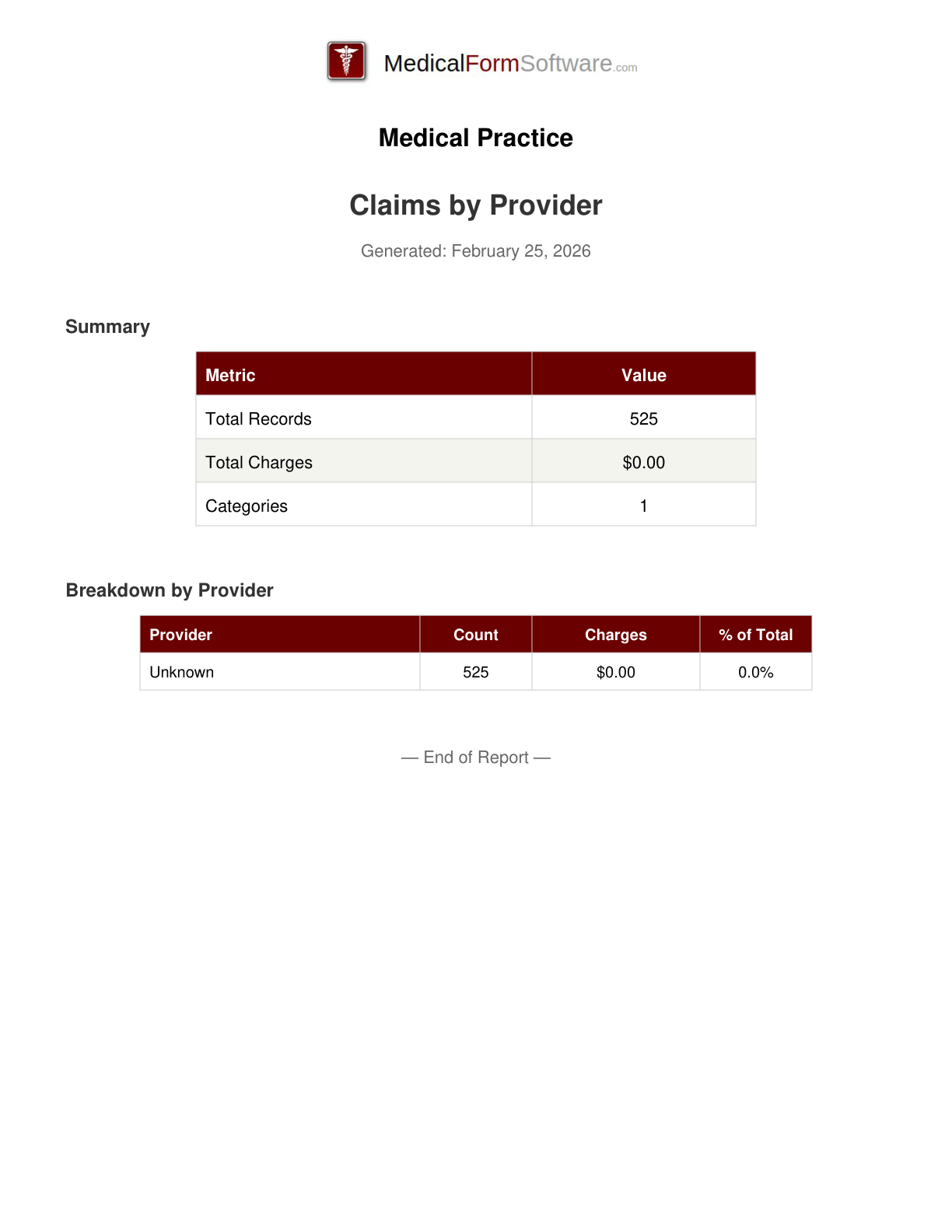
Grouped By Provider
Report
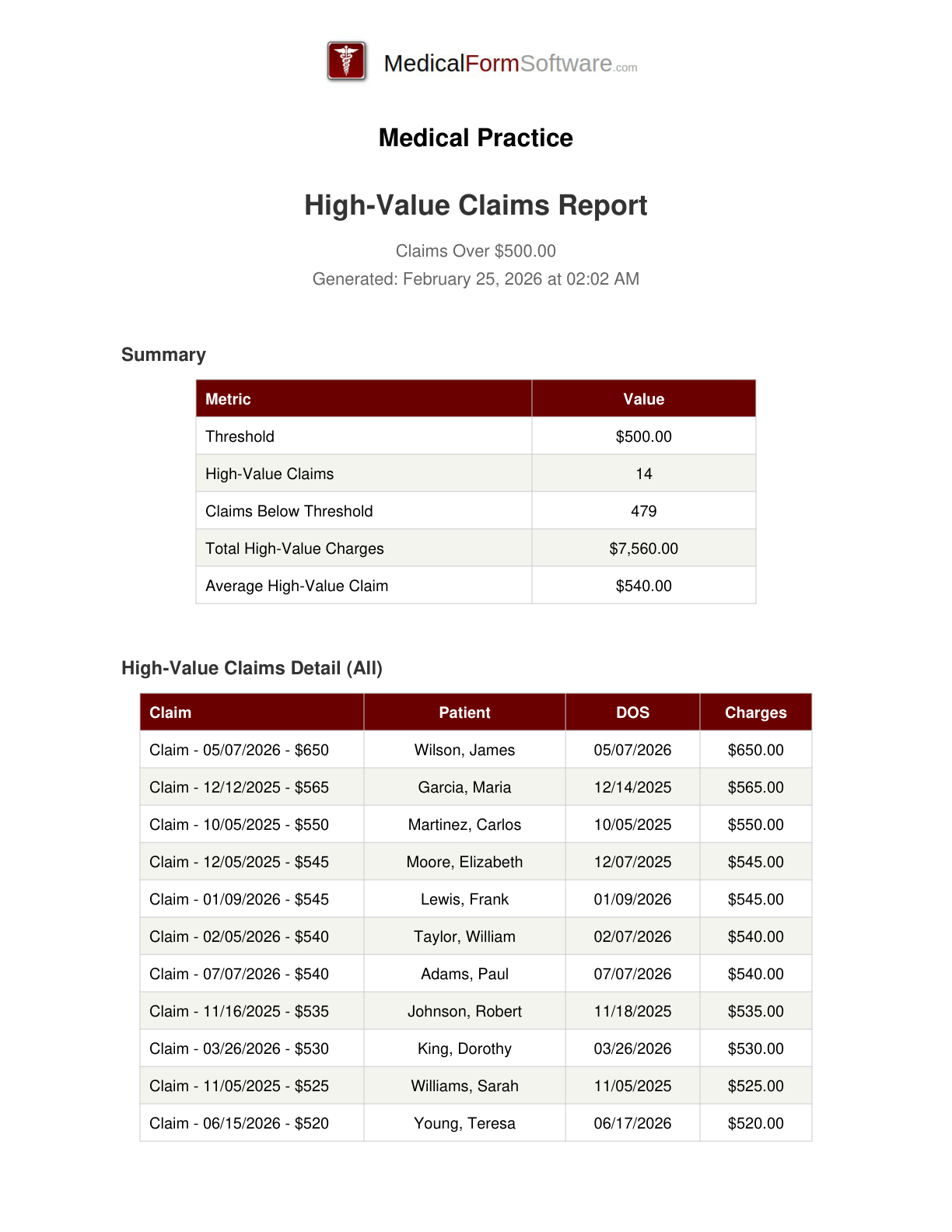
High Value Claims
Report
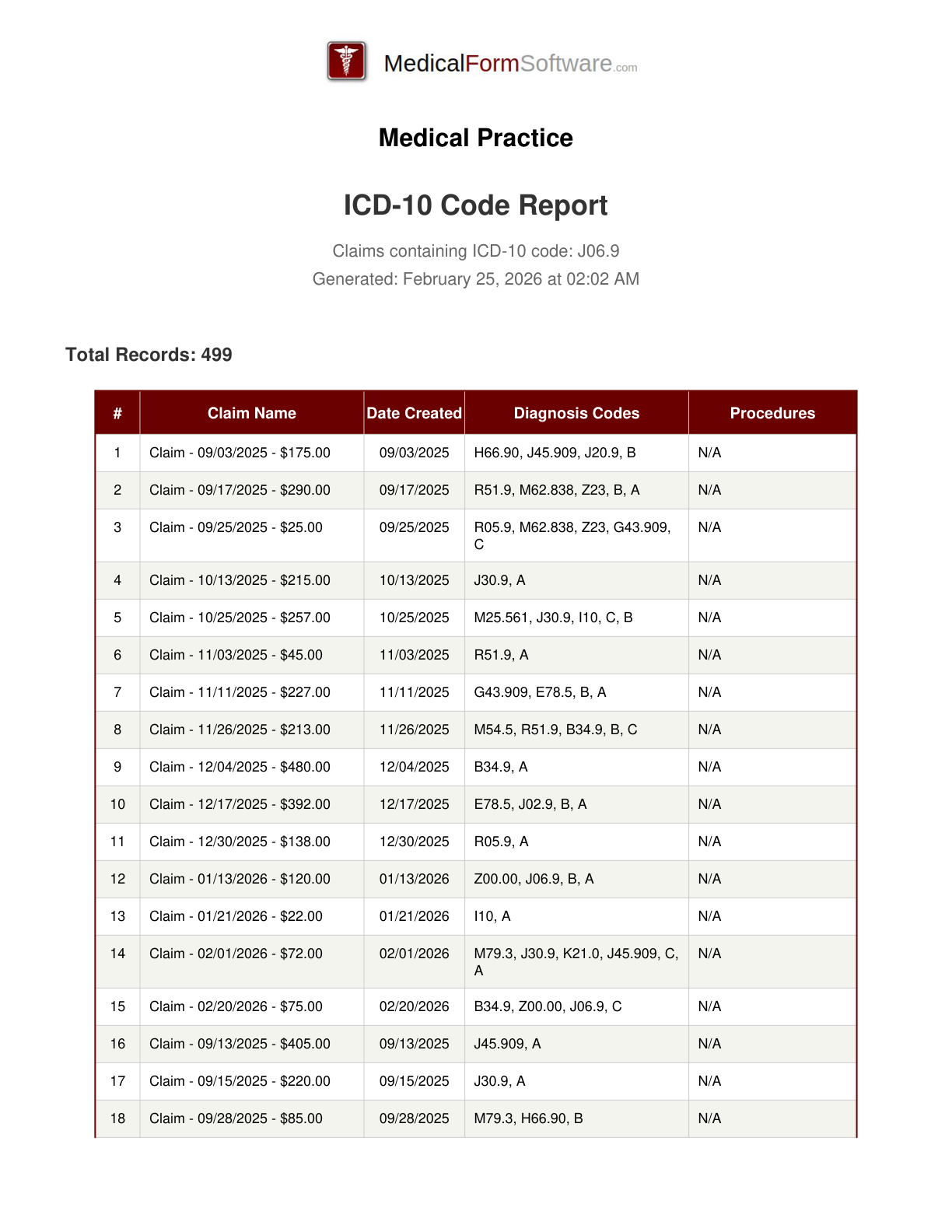
ICD10 Analysis
Report
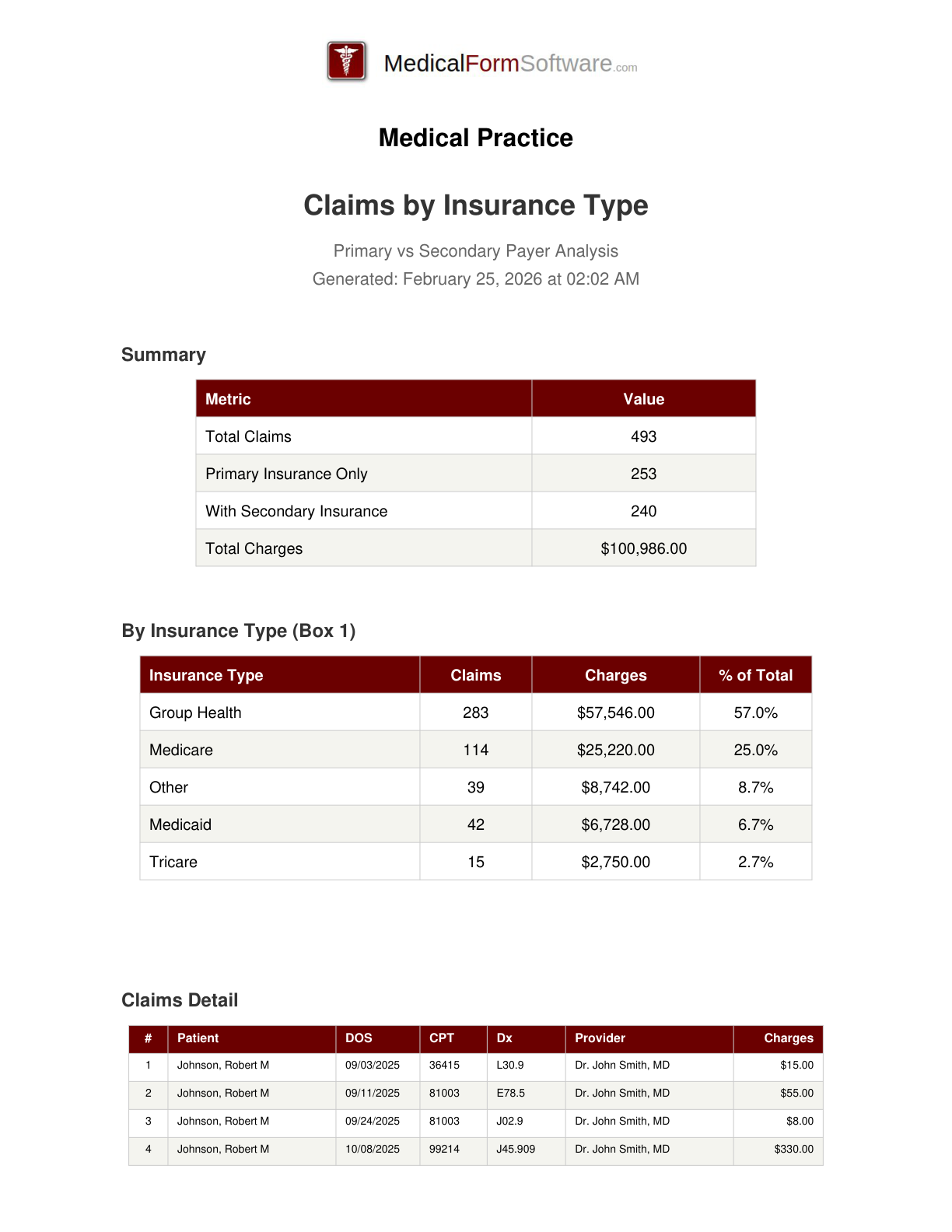
Insurance Type
Report
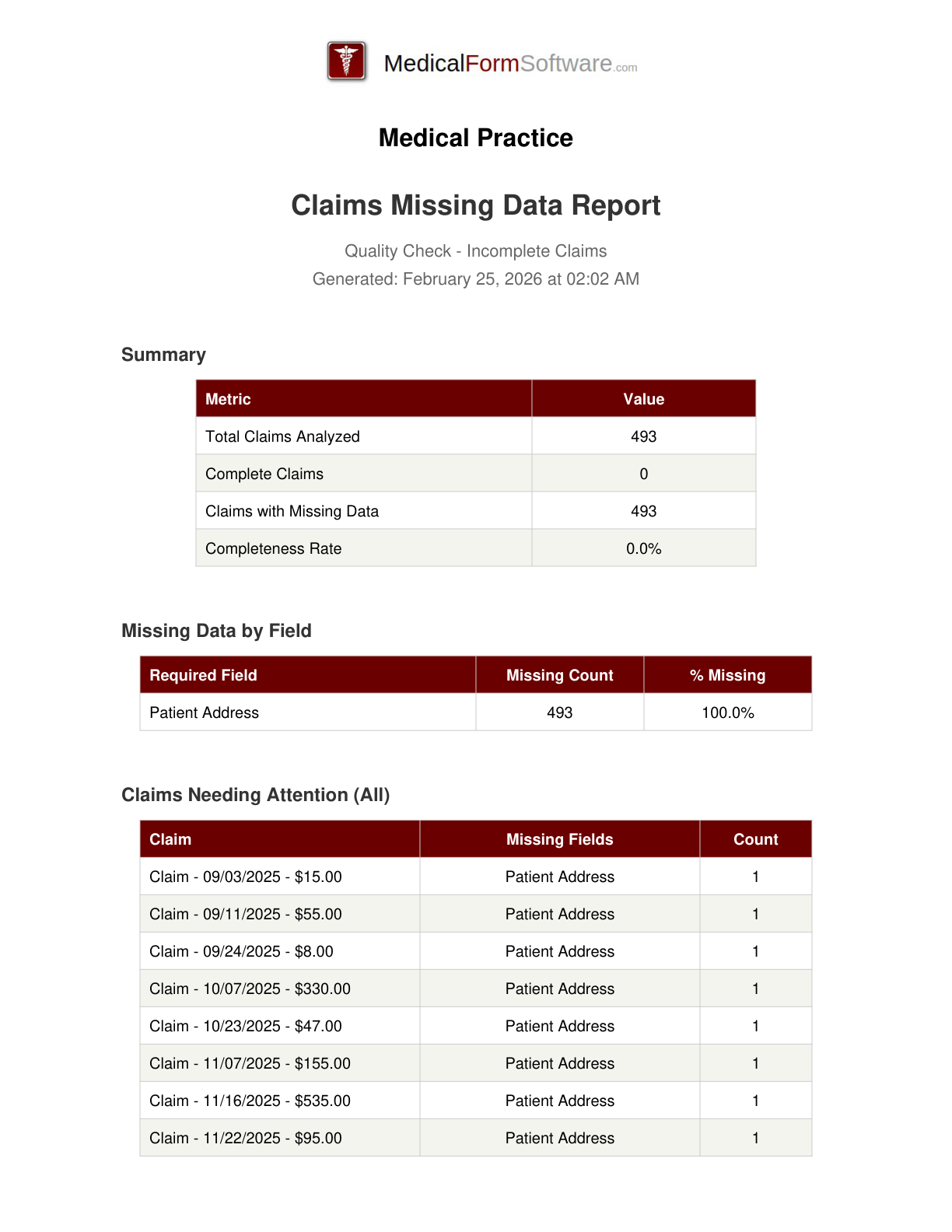
Missing Data
Report
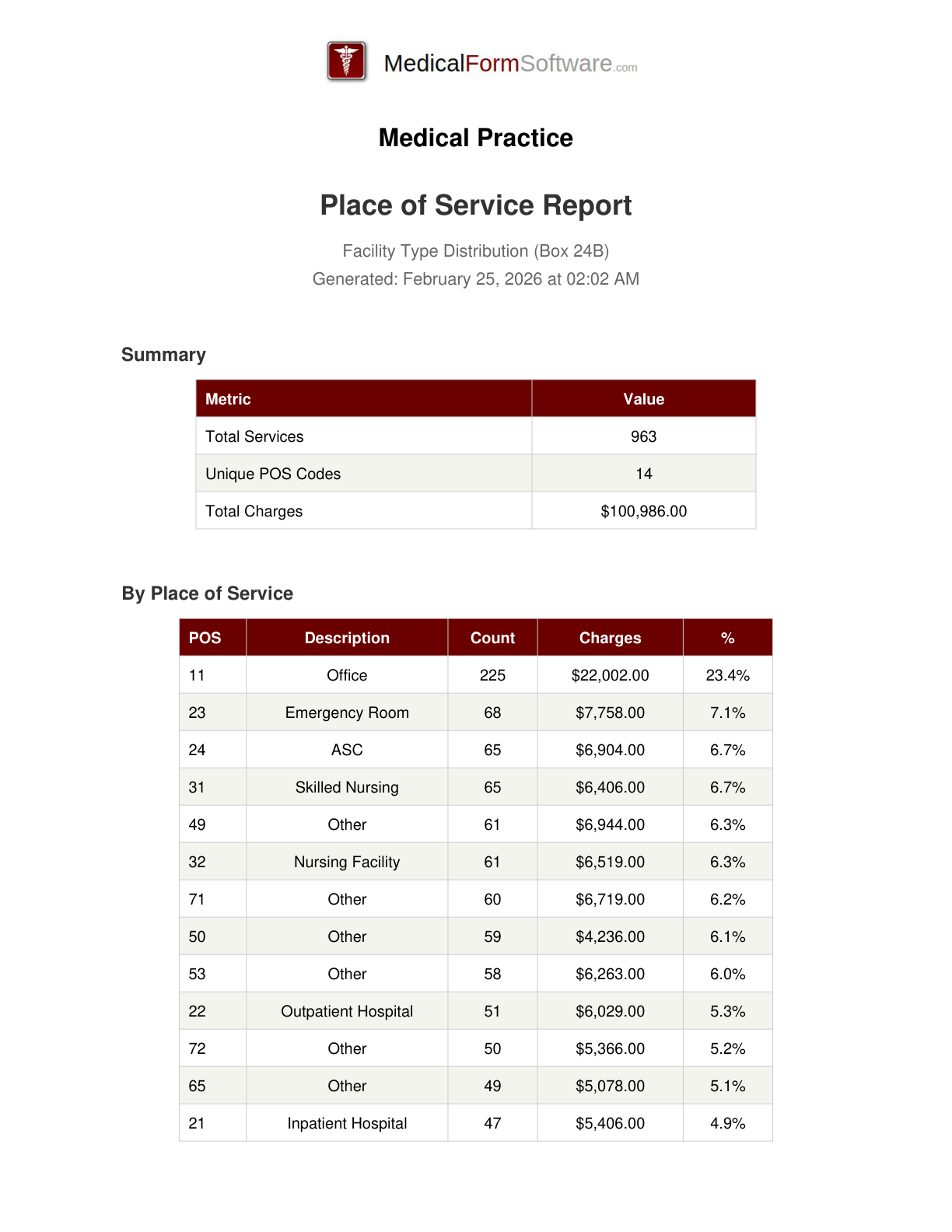
Place of Service
Report
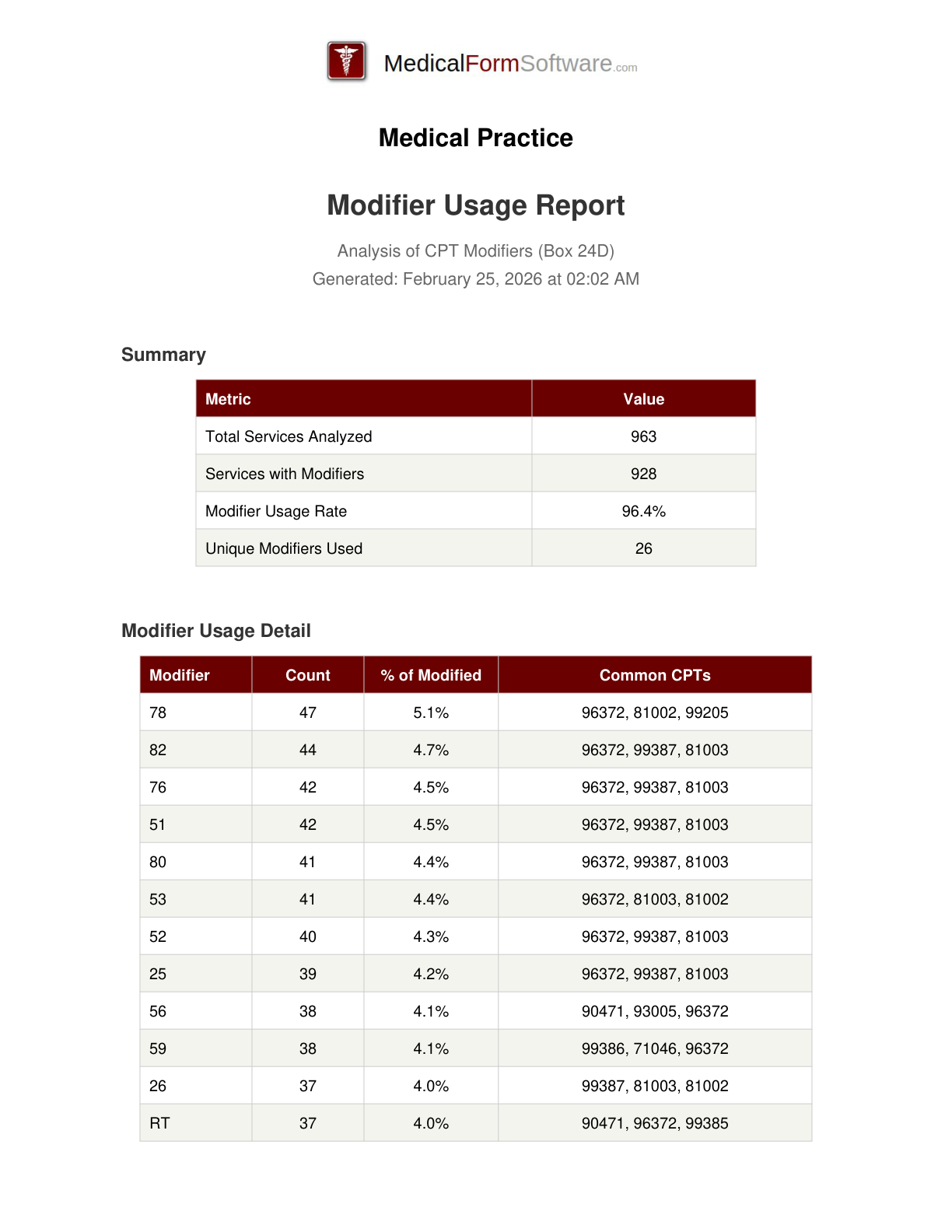
Modifier Analysis
Report
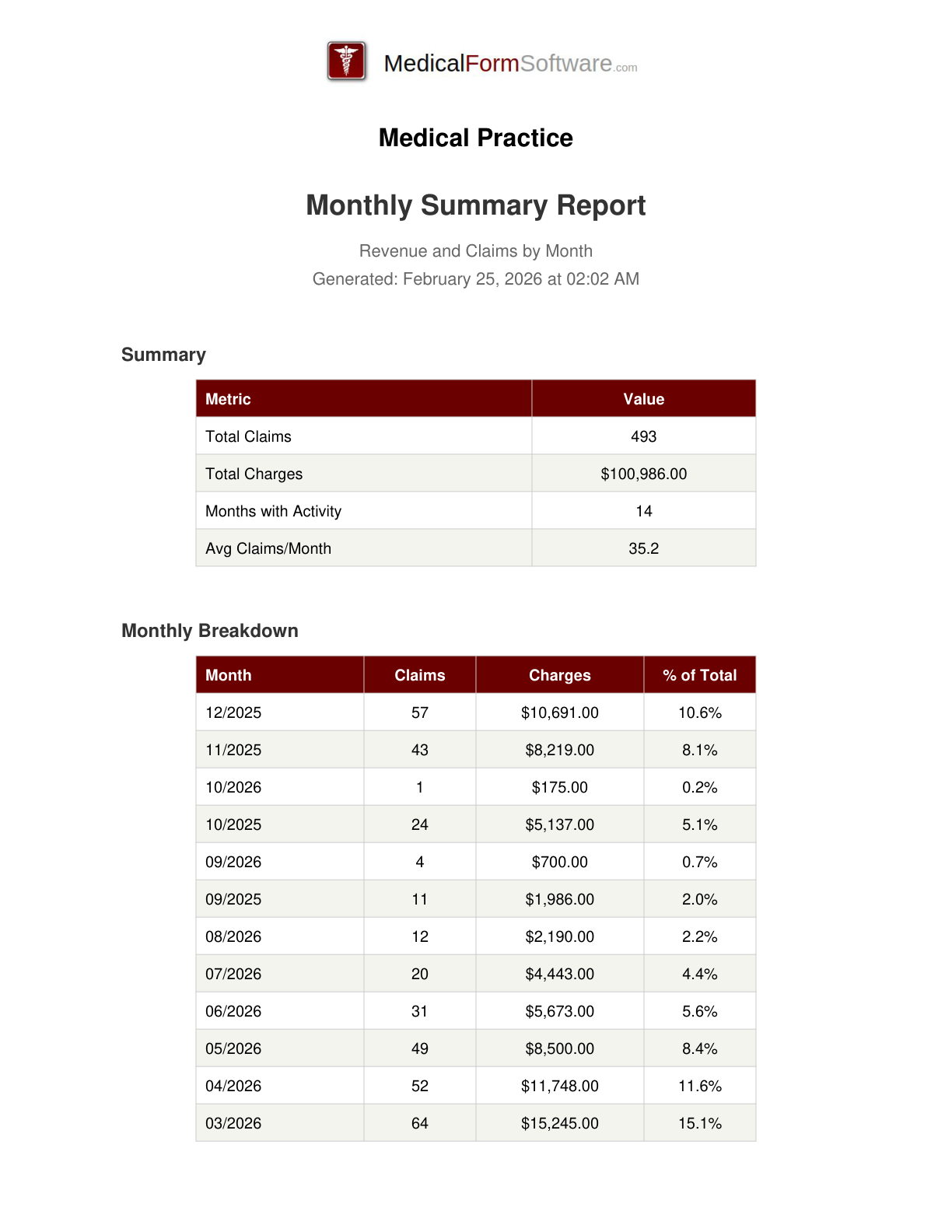
Monthly Summary
Report
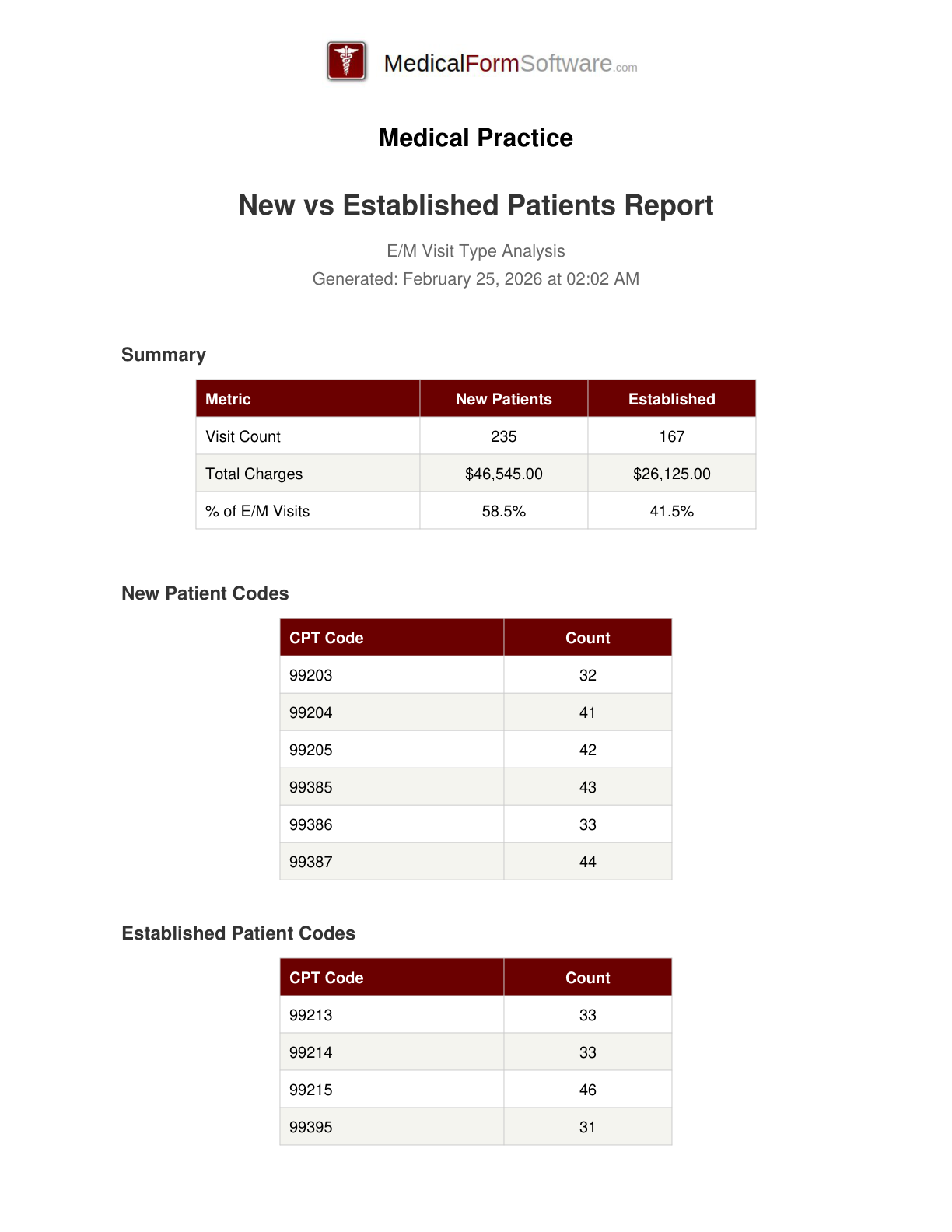
New vs Established
Report
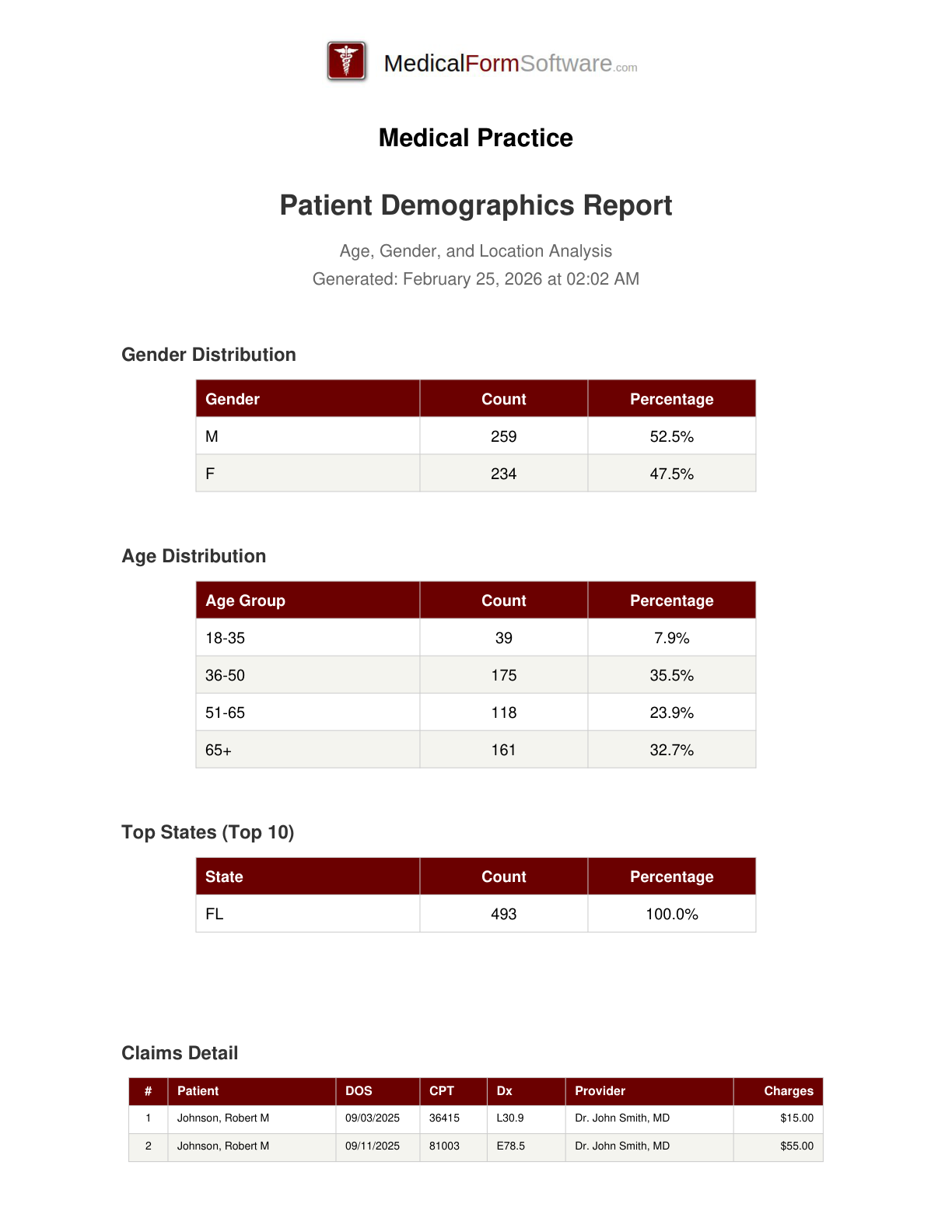
Patient Demographics
Report
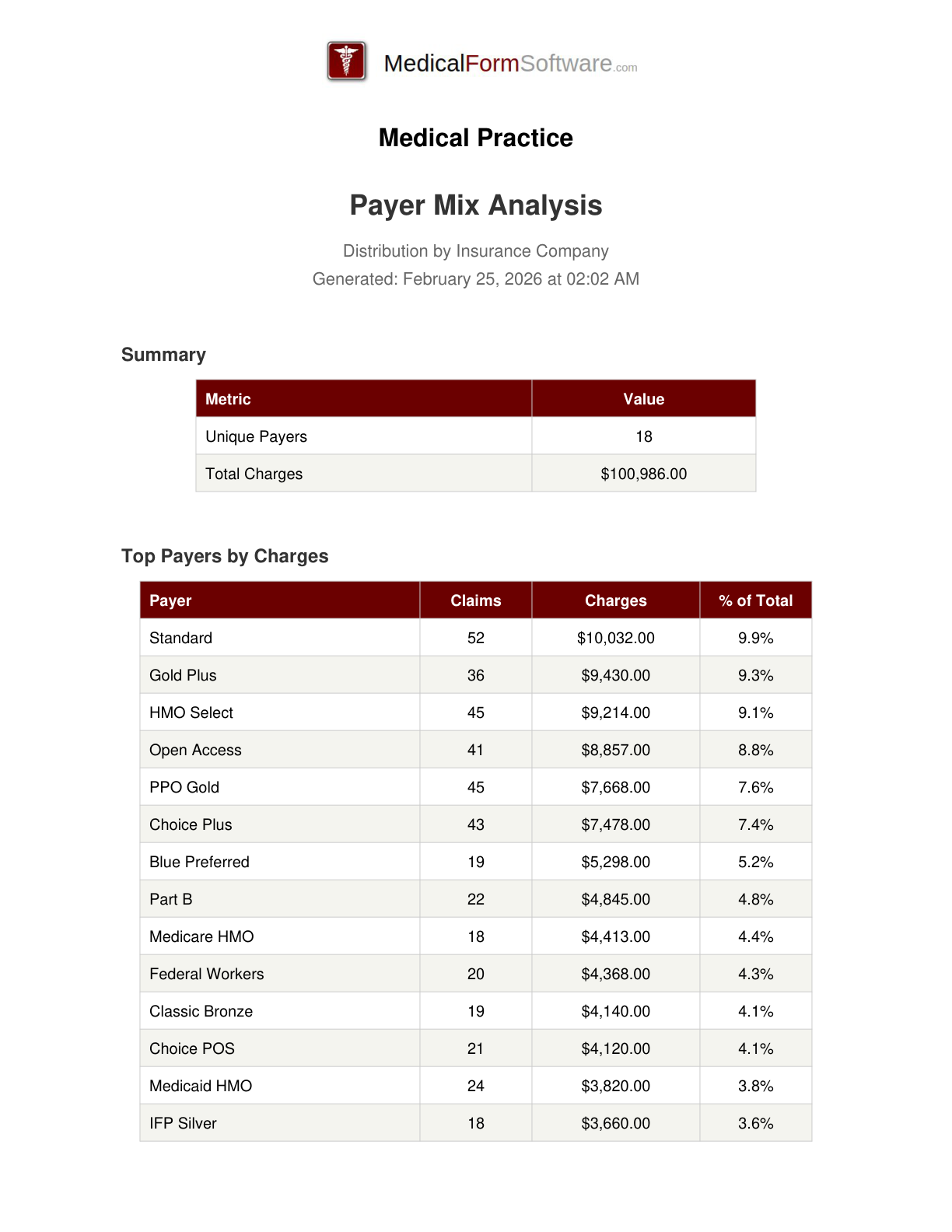
Payer Mix
Report
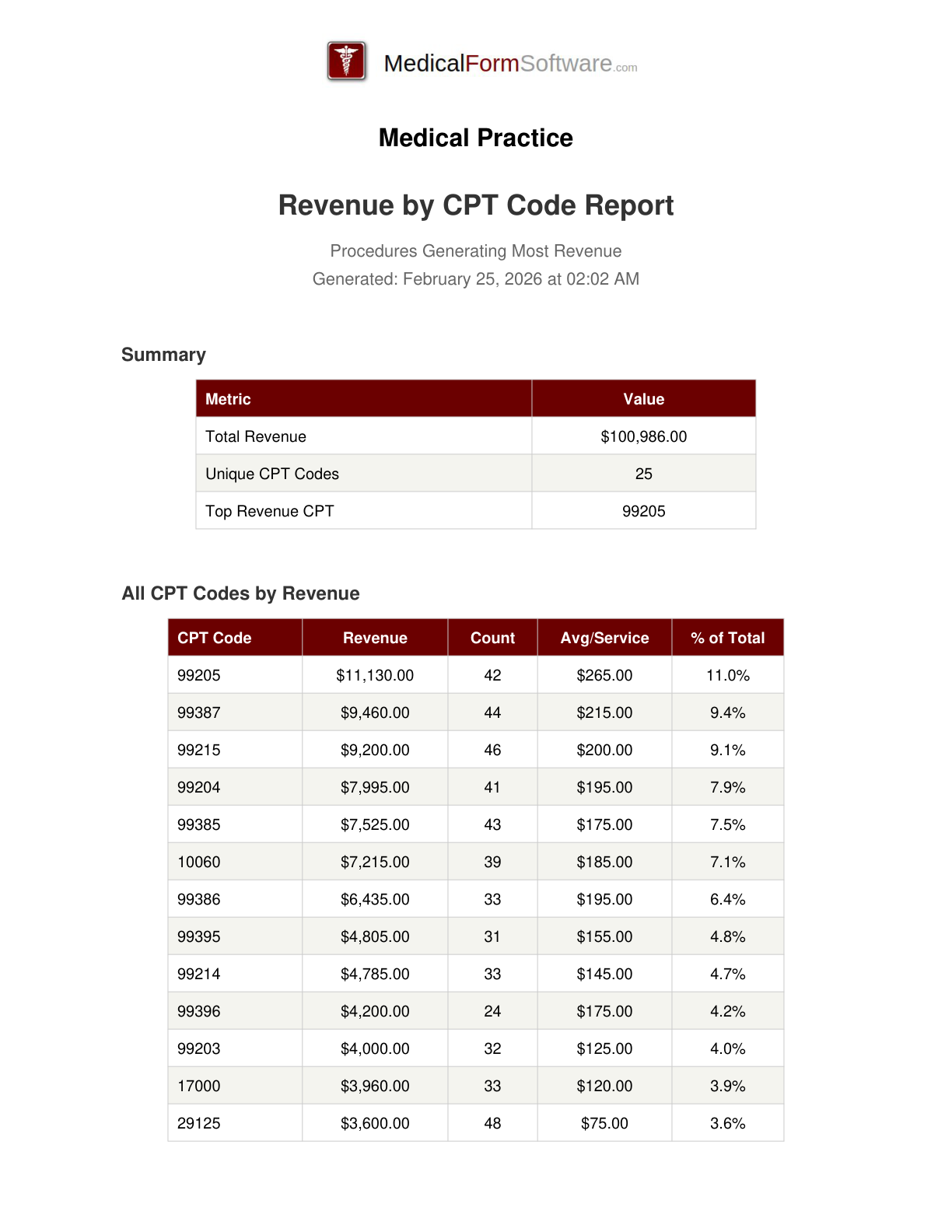
Revenue By CPT
Report
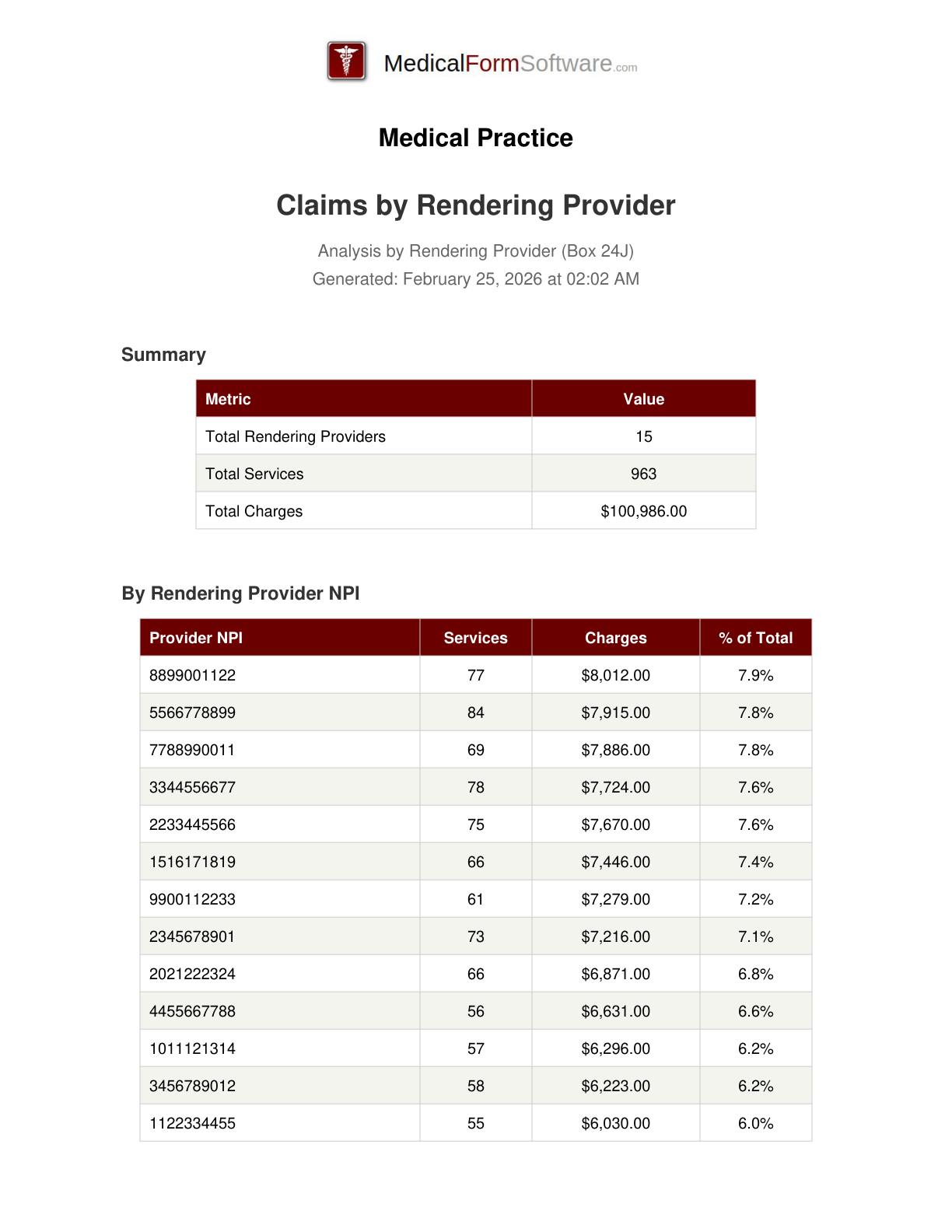
Rendering Provider
Report
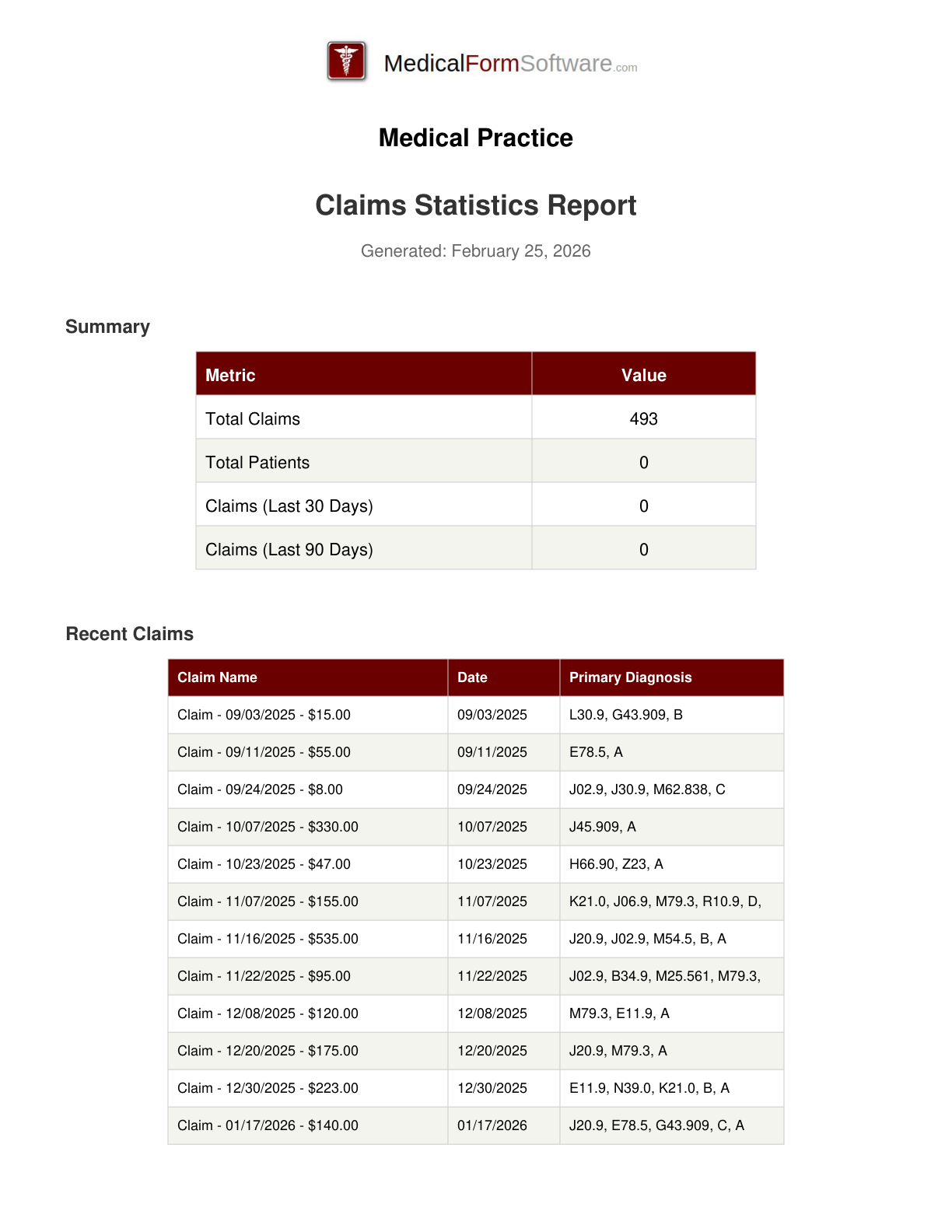
Practice Statistics
Report
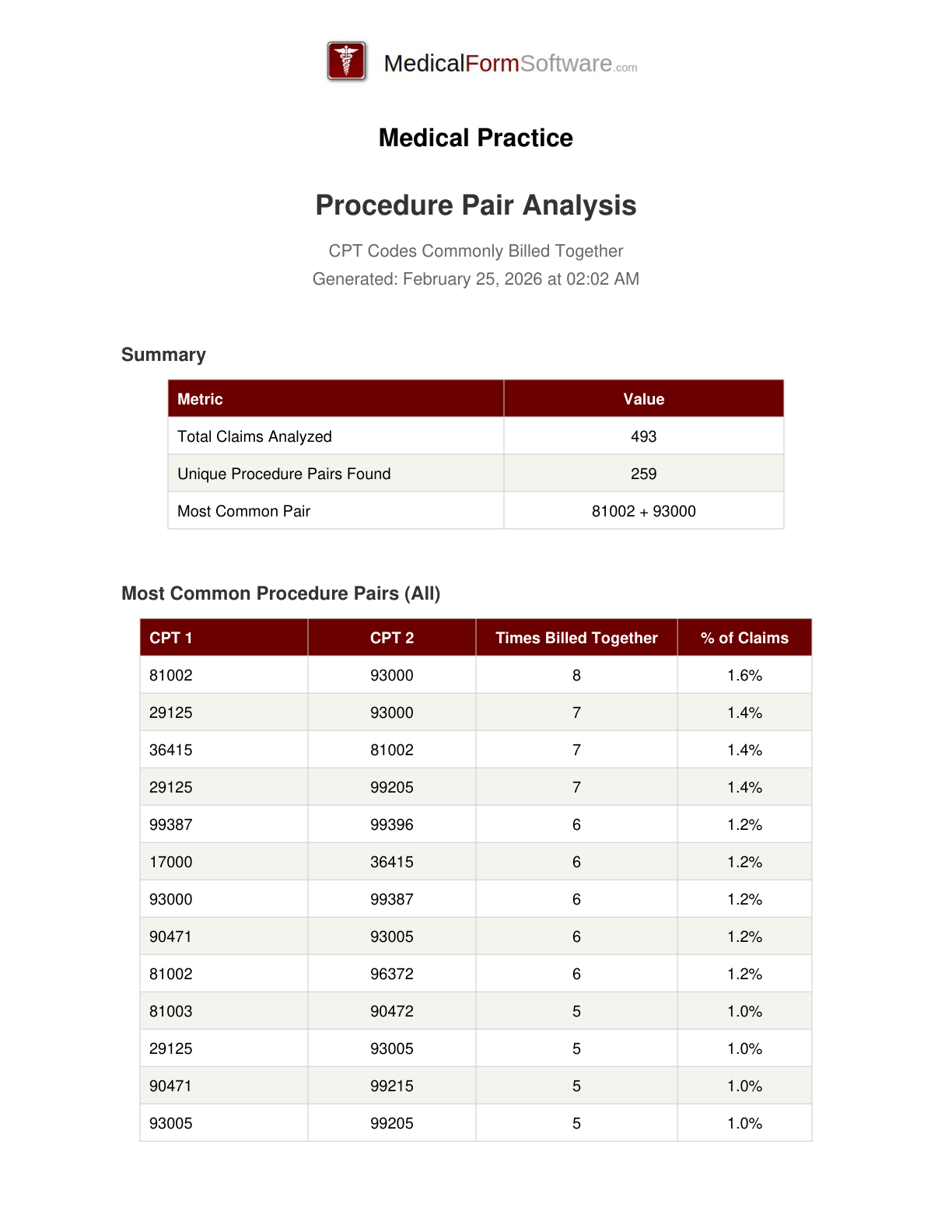
Procedure Pairs
Report
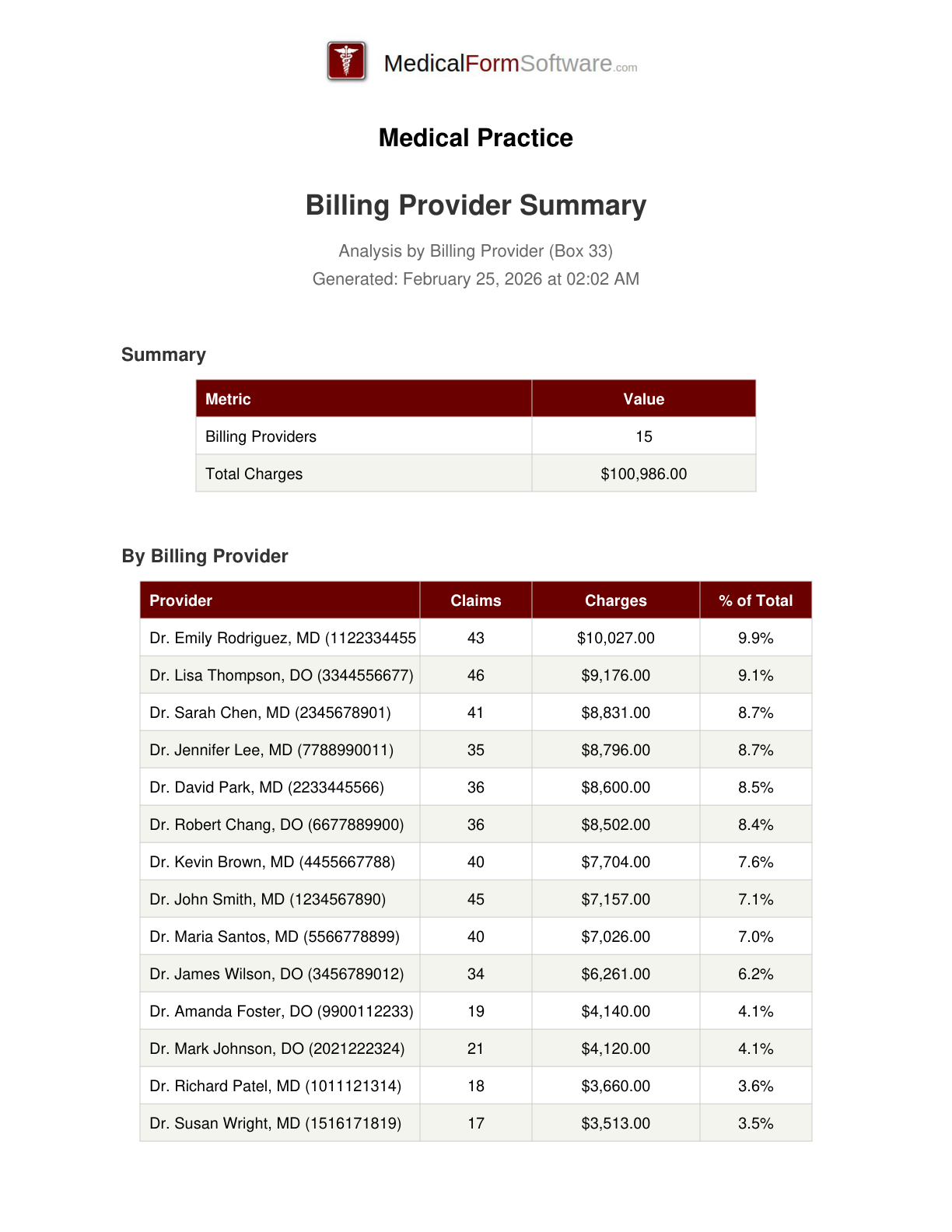
Provider Summary
Report
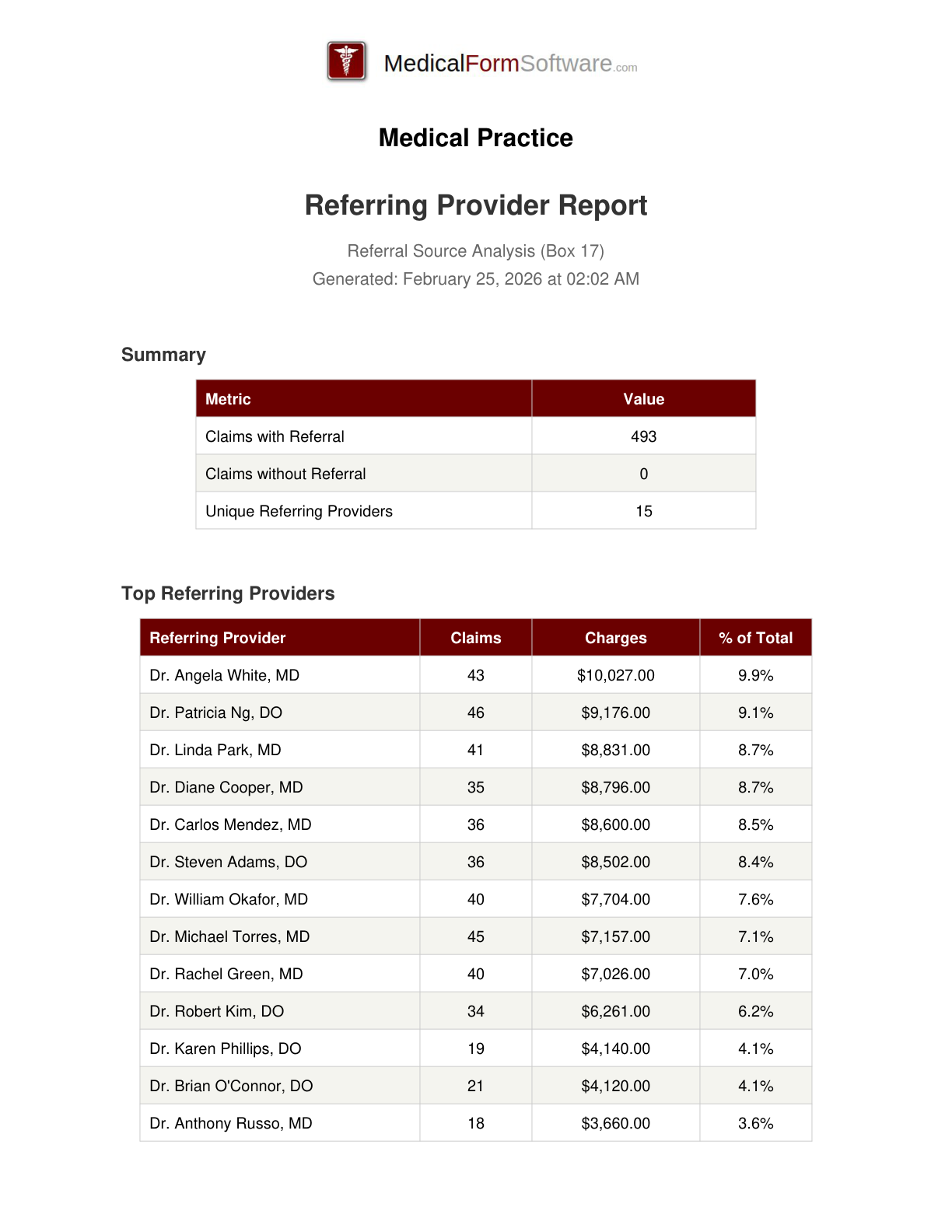
Referring Provider
Report
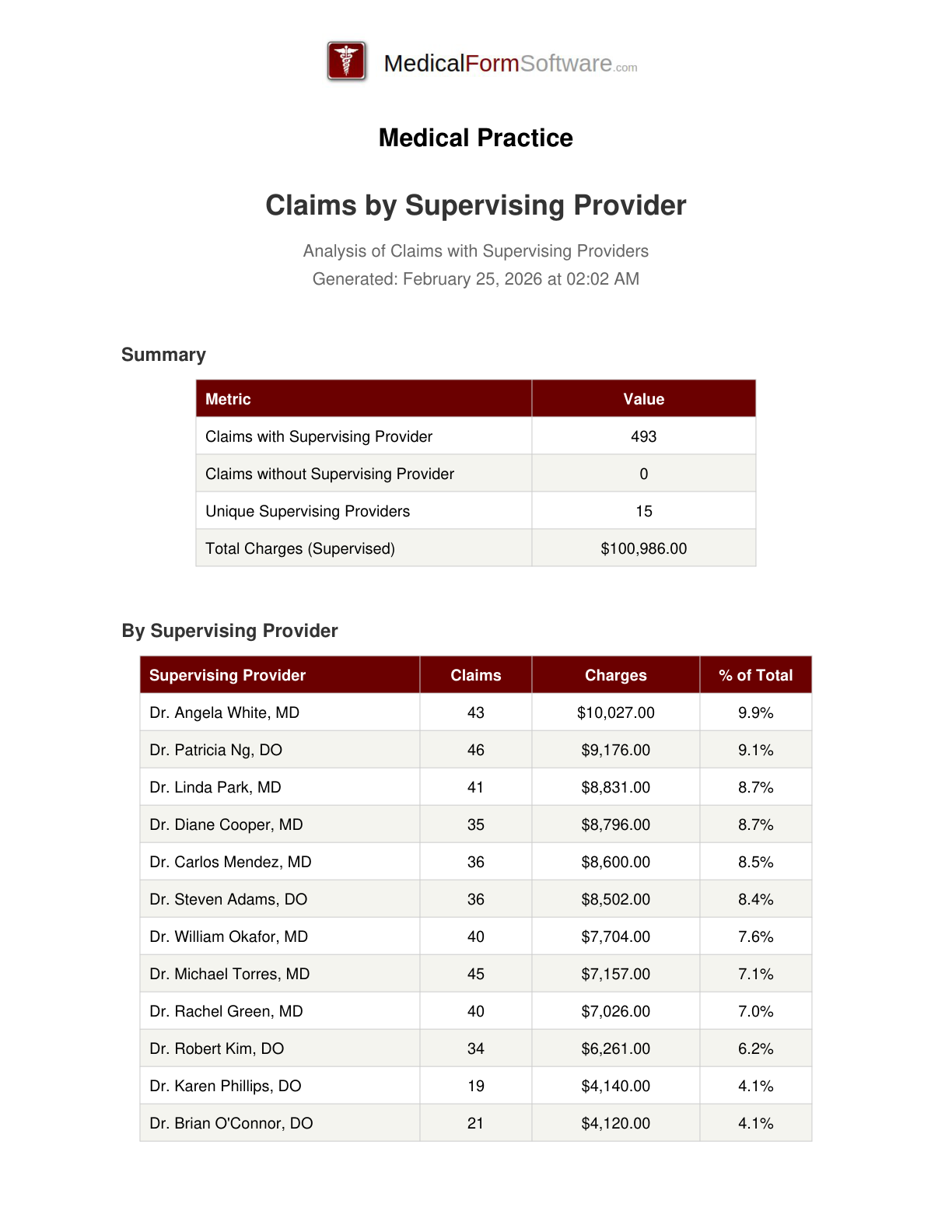
Supervising Provider
Report
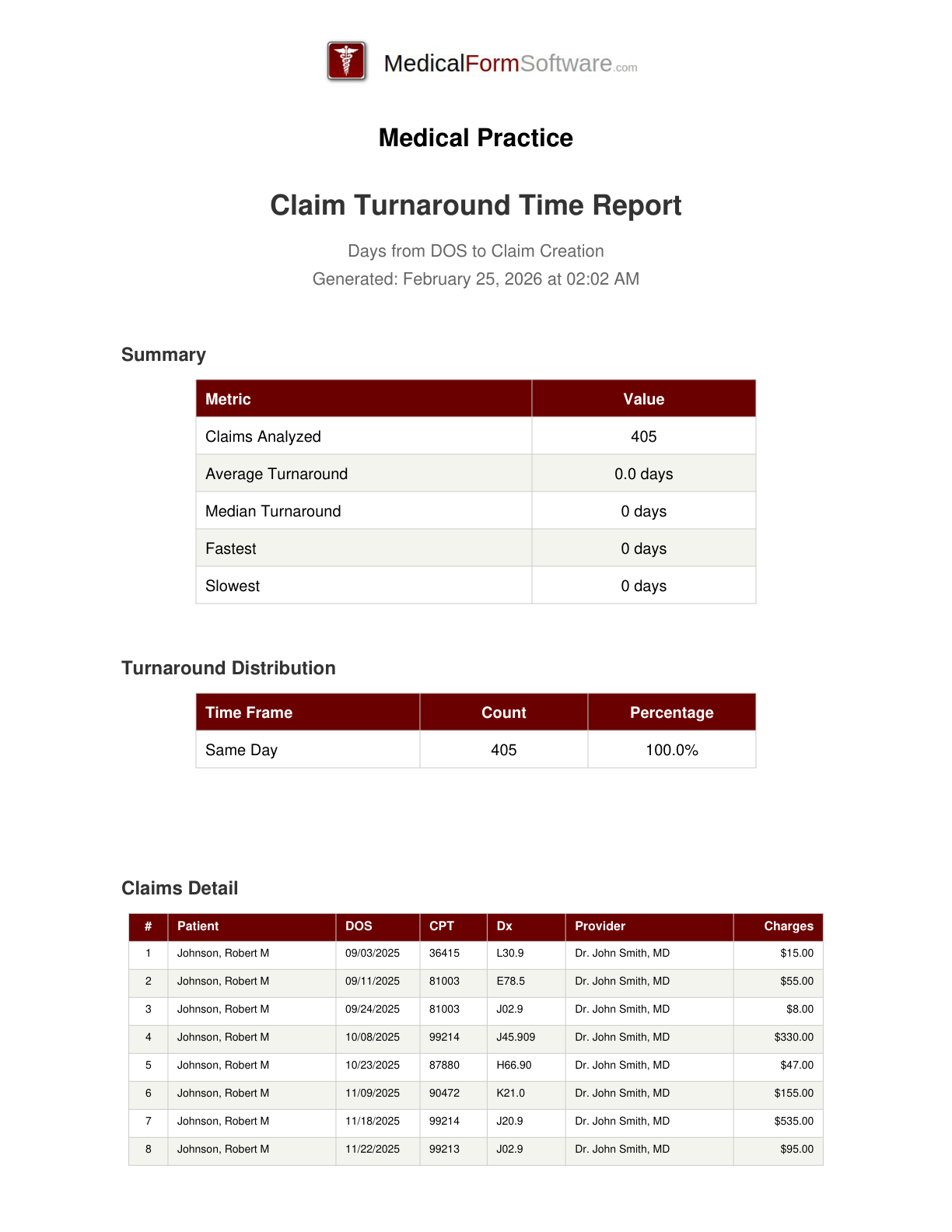
Turnaround Time
Report
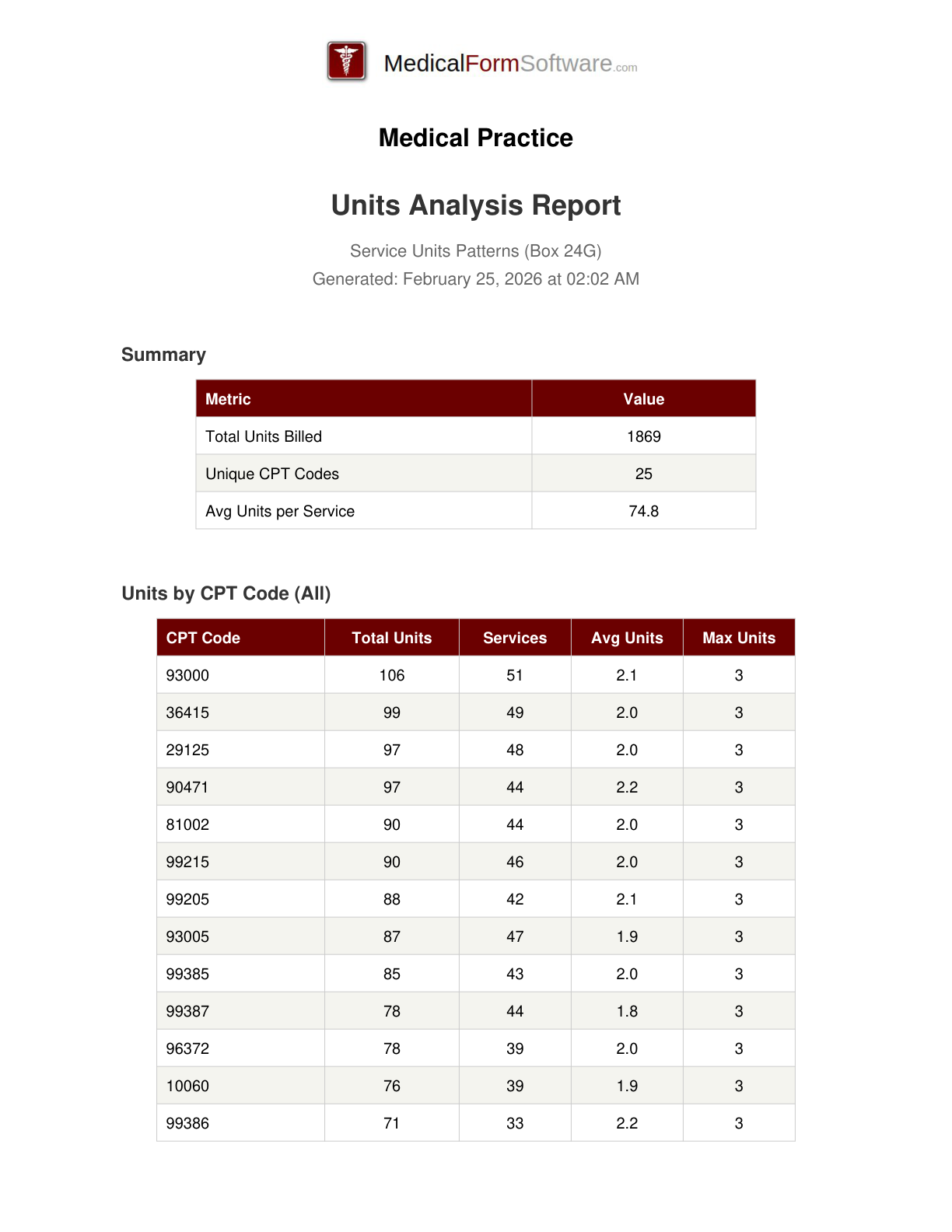
Units Analysis
Report
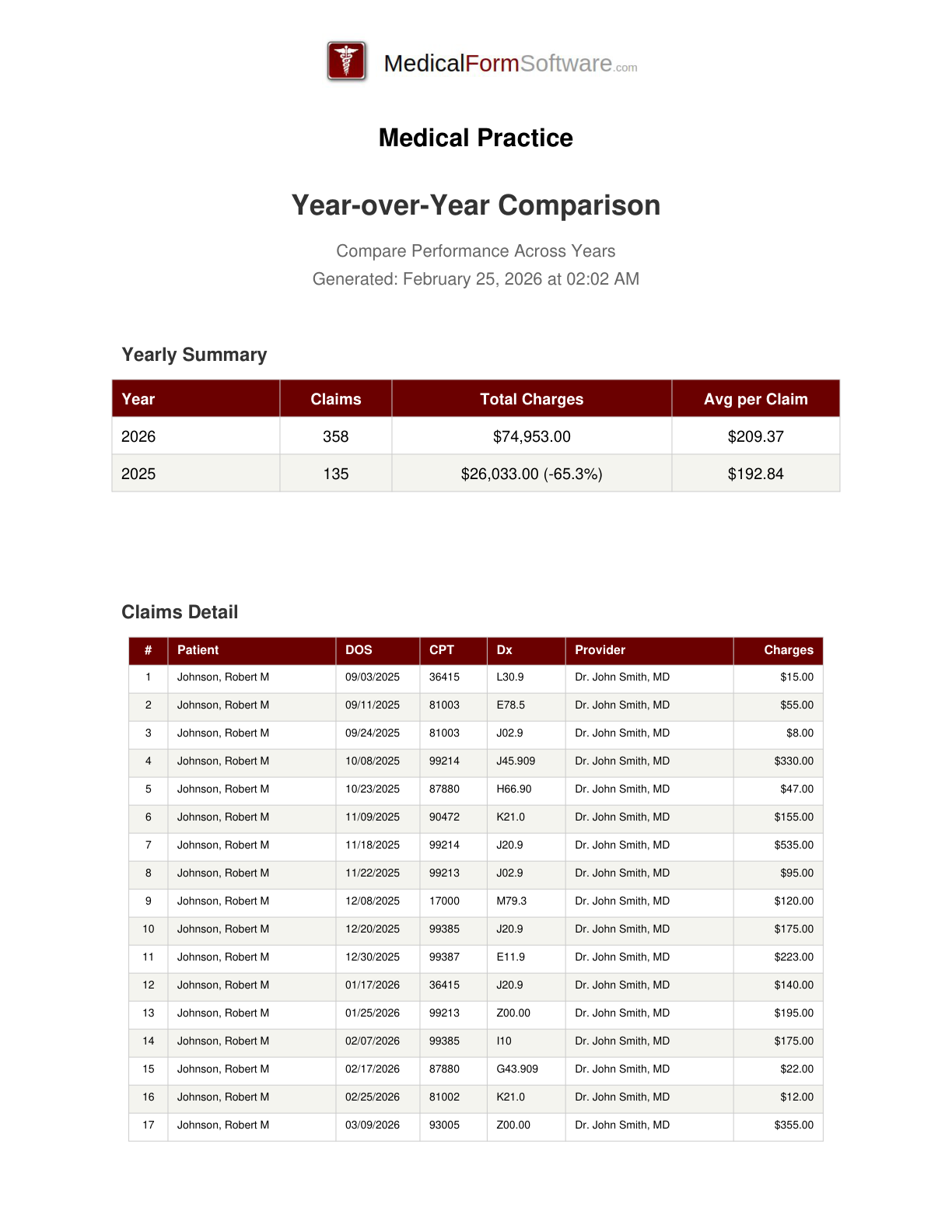
Year Over Year
Report





























